Piriformis Syndrome: It’s Not About the Tennis Ball
 Here we go. I believe the common treatment protocol for piriformis syndrome is not addressing the real issue. I understand this may stir some clinical debate, but as a PT who treats the cause of pain and not the area of pain, it doesn’t make sense to just treat the piriformis muscle. Currently, stretching, manual therapy and ultrasound (hello 1975!) are the main-stays of treating this syndrome. But, clinically, I have consistently found a different reason for piriformis syndrome.
Here we go. I believe the common treatment protocol for piriformis syndrome is not addressing the real issue. I understand this may stir some clinical debate, but as a PT who treats the cause of pain and not the area of pain, it doesn’t make sense to just treat the piriformis muscle. Currently, stretching, manual therapy and ultrasound (hello 1975!) are the main-stays of treating this syndrome. But, clinically, I have consistently found a different reason for piriformis syndrome.
Before we go any further, if you have symptoms of sciatica it is important to have a differential diagnosis. Ensure your medical professional (MD, DO, PT, etc.) is clearing the spine first.
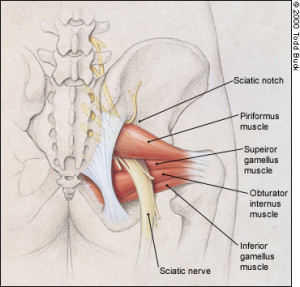
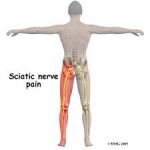
Compression of the sciatic nerve by the piriformis muscle, causing pain into the buttock and leg.
Piriformis syndrome was first described in a publication by Daniel Robinson, MD in 1947. It was an important article, giving an alternative explanation to sciatic pain. However, a pivotal piece of that article seems to have lost its way…
Common Symptoms of Piriformis Syndrome
- buttock pain that may or may not travel down the leg
- pain that is aggravated by sitting
- pain at the sciatic notch: a landmark where the nerve runs
Popular Treatments for Piriformis Syndrome
- Releasing the piriformis muscle via manual therapy or massage. This usually entails digging an elbow or fist into the painful muscle. Read below for further explanation.
- Stretching the piriformis. What if the muscle is long and taut and not short and thick? In general, it is usually not a length issue.
- Ultrasound. Honestly, I’ve used ultrasound maybe 10 times in my entire career. I’m in my 9th year of clinical care. You can see how important I think it is.
- Botulinum toxin injections to relax the hypertrophic piriformis muscle. Research is inconclusive about the long term effects.
- Surgery. Yes, actually cutting the muscle to take pressure off the nerve. This seems a little drastic, especially if not necessary.
As stated above, one of the common treatments for this syndrome is to excessively dig into the painful muscle, trying to release any trigger points. Sometimes there are trigger points, but what I most often hear from patients is that someone is releasing pain over the sciatic nerve! It sends chills up my spine. Because the sciatic nerve runs under the piriformis, applying pressure to this area elicits intense buttock and leg pain. But then something magical happens. The pain fades away and the patient feels relief. It is not because the muscle is being released but because the pressure begins to cut of the neurovascular supply to the sciatic nerve. This is the same idea as sitting on a tennis ball (which always makes me cringe!) to “release” the muscle. Shutting off blood flow to the sciatic nerve is not the treatment answer. Figuring out WHY the piriformis is compressing the sciatic nerve is the KEY to treating this syndrome. Once again, I find the Gluteus Maximus (GMax) and Gluteus Medius (GMed) are just plain lazy.
Causes of Piriformis Syndrome
- Abnormal emergence of the sciatic nerve. Sometimes it will pierce through the piriformis muscle making it more vulnerable to compression. Research states this occurs ~20% of the time.
- Fibrosis or adhesions of the piriformis muscle from trauma.
- Myositis ossificans of the muscle from blunt trauma. Calcification of the muscle occurs. This is rare.
- Hypertrophy of the Piriformis Muscle. This is the most common reason. But, here’s the clinical question: why is there muscle hypertrophy?
Ok, let’s dive into some specifics to better understand why I don’t treat the piriformis when someone presents with piriformis syndrome.
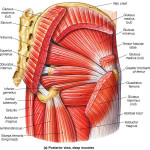
What is the Piriformis Muscle?
 Piriformis. It’s kind of of fun word to say. It is derived from the latin words pirum and forma. Pirum means pear, forma means shape. So, it is a long, triangular muscle that kinda sorta resembles a pear… a flat, squishy pear. It is an interesting muscle in that it can assist with hip internal rotation when the hip is flexed (in front of you) and with external rotation when the hip is extended (behind you). It will also assist with abduction (raising the leg to the side). It is a muscle that protects the sciatic nerve as it starts to travel down the leg, acting like a sling from the sacrum to the greater trochanter on the femur. Notice that the piriformis is an assistant…to all of the motions. And, clinically, I see it try to take on an entirely new motion: extension. This sets the muscle up to be bulky, hypertrophic and dysfunctional.
Piriformis. It’s kind of of fun word to say. It is derived from the latin words pirum and forma. Pirum means pear, forma means shape. So, it is a long, triangular muscle that kinda sorta resembles a pear… a flat, squishy pear. It is an interesting muscle in that it can assist with hip internal rotation when the hip is flexed (in front of you) and with external rotation when the hip is extended (behind you). It will also assist with abduction (raising the leg to the side). It is a muscle that protects the sciatic nerve as it starts to travel down the leg, acting like a sling from the sacrum to the greater trochanter on the femur. Notice that the piriformis is an assistant…to all of the motions. And, clinically, I see it try to take on an entirely new motion: extension. This sets the muscle up to be bulky, hypertrophic and dysfunctional.
What is the Sciatic Nerve?
The sciatic nerve is a large nerve that travels down the back of the leg to innervate the hamstrings, part of the adductor magnus, the lower leg and foot muscles. It is a thick cord of nerve fibers, receiving input from L4, L5, S1, S2, and S3. (Now you can see the importance of clearing the spine first!) The nerve travels to the back of the leg behind the piriformis muscle and courses down the center of the thigh. Around the knee, it breaks into 2 branches: the tibial nerve and common peroneal nerve. It is a long, important nerve that, when irritated, causes pain in the buttock and leg.
What is Muscle Hypertrophy?
 Hypertrophy of muscle occurs as an adaption to heavy load or use. It is an increase in the size of the muscle fibers and cellular components; the cross-sectional thickness actually increases. Hypertrophy is a sign that the muscle is receiving A LOT of neural input to make the muscle contract. Can you imagine if your piriformis had muscle hypertrophy and to decrease it, someone said: “Just stretch.”
Hypertrophy of muscle occurs as an adaption to heavy load or use. It is an increase in the size of the muscle fibers and cellular components; the cross-sectional thickness actually increases. Hypertrophy is a sign that the muscle is receiving A LOT of neural input to make the muscle contract. Can you imagine if your piriformis had muscle hypertrophy and to decrease it, someone said: “Just stretch.”
Back to the question: Why is there hypertrophy of the piriformis muscle? Mr. and Mrs. GMax and GMed have decided to not pull their weight! This is not the fault of the piriformis. Our bodies are incredibly smart and will compensate however needed. If GMax is not doing its job in all three planes (extension, abduction and external rotation), the piriformis says: “Ooh, pick me! I will help you!” If the GMed (main abductor) is lazy, the piriformis, once again, begins to work harder. So, can you see that simply releasing the piriformis, stretching the piriformis and moving ultrasound gel over the piriformis will not fix the real problem? Teaching our glutes how to work is the answer! In addition, making sure the main rotators of the hip (gemellis, obdurators, quadratus femoris) are doing their job too.
Above I mentioned that Dr. Robinson originally described piriformis syndrome in 1947. And, in his paper he also found that gluteal atrophy was more likely and a cardinal criteria of piriformis syndrome. Let me re-phrase that. Atrophy of the glutes is associated with piriformis syndrome. Hmmm…
If the piriformis is the only area getting treatment, the syndrome will never truly resolve. It is imperative to teach the glutes and hip rotators how to work in order to decrease the load on the piriformis.
Increased work load on the glutes = decreased work load on the piriformis
Decreased work load on the piriformis = decreased hypertrophy
Decreased hypertrophy = decreased compression on the sciatic nerve
Decreased compression on the sciatic nerve = pain resolution!
I hope this makes sense now.
A Research Case Study
 A 28 y.o. competitive cyclist had an MRI showing hypertrophy of the left piriformis. He was given a prescription of massage, stretching and botulinum toxin injections. This combination did not work, so the cyclist had 2/3rds of the piriformis cut
A 28 y.o. competitive cyclist had an MRI showing hypertrophy of the left piriformis. He was given a prescription of massage, stretching and botulinum toxin injections. This combination did not work, so the cyclist had 2/3rds of the piriformis cut
What muscles do I consistently educate about in my blogs, especially when it applies to cyclists and runners? The weakness of the glutes…something to ponder.
© 2015 and Beyond! ALL BLOG CONTENT at duncansportspt.com by Lori Duncan PT
BLOG TALK PODCAST:
Blog Talk – Piriformis Syndrome
ABOUT THE AUTHOR
 Lori Duncan, DPT, MTC, CPT is a respected Physical Therapist, Manual Therapist and Pilates instructor in Lafayette, CO. Lori is passionate about preventive physical therapy and education and is a nationally recognized presenter. She can be reached at [email protected]. You can also follow Duncan Sports Therapy + Wellness on Facebook & Instagram for more free tips and information.
Lori Duncan, DPT, MTC, CPT is a respected Physical Therapist, Manual Therapist and Pilates instructor in Lafayette, CO. Lori is passionate about preventive physical therapy and education and is a nationally recognized presenter. She can be reached at [email protected]. You can also follow Duncan Sports Therapy + Wellness on Facebook & Instagram for more free tips and information.
References
Fouasson-Chaillou A, Dubois C, Dauty M. Piriformis syndrome diagnosis: on two professional cyclists. Ann Phys Rehab Med. 57(4):2014;268-274.
Papadopoulos EC, Khan SN. Piriformis syndrome and low back pain: a new classification and review of the literature. Orthop Clin N Am. 35:2004;65-71.


I just love your insight to the athlete, you just really get us!!
So, what is the answer?
What do we do to resolve the pain
Hi Carole. You find the exercises that feed into getting the good glutes to activate. That’s the ticket.
Thank you so much for this information. I have been suffering with Piriformis syndrome for 22 years now (since an injury when I was 14!). I have undergone therapy, which did help, but I was not focusing on strengthening glute muscles, only my posture! I appreciate your sharing your knowledge, and I will be now focusing more on my glutes. It just makes so much sense. The tennis ball just never made sense as far as any permanent solution to the pain, and part of me has just accepted that I will deal with this pain for the rest of my life… …Well, until I read your article. <3 Thank you.
Where is the answer here…? If the answer is lazy glutes then why do you not provide exercise or a link that you feel is good for activating glutes….?
Hi Sandra,
Yes that is the answer. And, I have a blog talk that does address a few exercises. My blogs are not meant to be treatments but advice on getting the correct treatment. You should reach out to a local PT for some expert advice.
Thank you Amy! I feel honored to work with all you amazing athletes.
Lori, post hip replacement surgery, why is piriformis tight, or is it? And why does stretching piriformis cause groin pain? Ps, six weeks out from dual mobility cup, anterior total right hip. Doing bridges, sit to stand, stationary clams
Hi,
Surgery shuts off stability muscles. So, the piriformis is likely just trying to take over. The stretch of the piriformis is likely not causing the joint pain, but the position of the hip. Do some glute squeezes on your stomach to have a pain free glute contraction. Bridges usually aggravate this condition. Clams ok.
This perspective is dead on from my own experience. I love to cycle but at certain times of the year when it’s hard to get time combined with lots of driving I get the piriformis syndrome and the stretching and tennis ball techniques never work, it’s always back to the bike and it works it out everytime.
Hi Rick,
Thanks! I’m glad you get relief from using your glutes on the bike. 🙂
Hi Lori,
I don’t understand this. Doesn’t bicycling (as it’s pointed out in the case study at the end of the articles) contribute to problems with weak glutes? Or is this a case where Rick was doing absolutely nothing with his legs during certain times and then the bicycling at least contributed something to help with that? I am a cyclist as well and have this type of issue with my piriformis. I was prescribed clam shell exercises that haven’t helped yet, but will keep at it. For the record, I 100% believe that my issue started when I tried some at-home yoga for the first time that forced some stretches that threw my legs into chaos. So I am nervous about further stretching (which also doesn’t help) and at least understand the benefit of strengthening the glutes.
Hi Sean,
Sorry for the delay. Just seeing this. NO, no. Cycling does not and should not turn off glutes. We know from EMG studies that the glutes are highly dominant in cycling (along with with the quad, HS, calf, ant tib). So, yes, work on those glutes!!
So if I need to increase workload on the glutes, then what are the best exercises. Heavy squats are out of the question. I have tried tennis ball on the knots for months. I had some relief when I focused on contracting hip adductors and hamstrings and glutes with bridges. Also, my TFL’s always cramp up. I have the “no butt syndrome”, and probably under developed hamstrings every since my back injury 6 years ago. What do you recommend for training the glutes, without putting too much compression on lower back. I figured that the traditional slanted leg press puts too much pressure on spine, and doesn’t fully engage the glutes. Any thoughts?
Thanks
Hi Cory,
Thanks for your question. In general, it is easiest and most effective to train the lazy muscles “off the ground”. We call it non-weight bearing in PT. That said, I use two main exercises in the clinic, one for glute medius and one for glute maximus. I wrote a post about it a few months ago (someone else had your same question). Here is the link…I hope it works. If not, you can search for “Top Two Exercises I use in the clinic”. Please let me know if they help!
Hi. I can’t find the link or where to search the top 2 glute exercises. I have been using the tennis ball and stretching and came across your article saying that this wasn’t a good idea and it makes perfect sense !! I am having severe pain in right glute and down along upper outer side of right calf.
Hi Diana,
Thanks for reading. Oh yes, please stop with the tennis ball. Here is the link. Find the good glutes!
https://www.duncansportspt.com/2014/09/glute-exercises/
I have been struggling to understand piriformis hypertrophy as well. This rationale makes perfect sense.. almost too obvious that it gets hidden in plain sight!
Great work, thank you so much for sharing your insight!
See if this works. Glute Exercises
I love your articles! Quick question though, what are your thoughts on acupuncture combined with yoga to get that little pear to heal up? I started getting acupuncture when I self-diagnosed the pain in my butt to be sciatica & felt some relief. After reading about the piriformis, I think it may be because of that. I love running but this is kind of putting a damper on my ability to run.
Thanks for the articles & hope to see a reply!
Hi Patrick,
Thanks for reading! I think acupuncture is always a great combination with PT to help with pain modulation. However, it will not help decrease the size of the piriformis. Only taking the load off the piriformis will really do that. Yoga, is excellent as well especially as a cross training exercise for running. Although the symptoms may seem that they will never go away, they really will if you find glute med and max. Stay patient and do some pool running (put old shoes on and strike the ground. I give this to patients all the time to keep the mechanics of the run going!)
Keep me posted!! Lori
Great article! I’ve had piriformis syndrome in my right leg since May, and suspected a couple of things, like increased neural input to the muscle causing it to involuntarily compensate for lazy glutes, that your article has now confirmed. Definitely explains why a single beer is enough to relieve a lot of my pain (alcohol being a CNS depressant). Is there anything more I can do besides the exercises and being actively ‘conscious’ in relearning to use the right muscles? From the sound of things, the atrophy of the piriformis muscle to its normal size/neural stimulation seems to be the best solution.
Hi!
Thanks for reading. I wish there was a magical answer, but finding the right muscles is the key. And that can take several weeks for your brain to say: “oh, you want me to use THAT muscle.” Ice and acupuncture can sometimes give relief, but sounds like you have that taken care of with a beer! Having the instrinsic abdominal muscles (transvere ab, internal oblique) efficient and active is very helpful too. They help stabilize the pelvis so the glutes can work optimally. Hope that helps and hope you get relief soon!
Lori, thank you SO much for this. I just wondered – you said stay patient, but do you have any thoughts on time frame? As well as doing my PT-mandated Figure 4 stretches, improving my core stabilisation, sitting less and ‘better’, and keeping active, I have been faithfully doing 20 clams, on each side, daily since August/September. (Position checked by multiple PIlates instructors so I am confident I’m doing them correctly). I have seen steady improvement but had another big flare-up this month … Possibly caused by a week of too much sitting.I just wondered if that kind of time-frame seems ‘normal’ to you or if I should look to kick things up a notch? Is it possible that I’m strengthening the glutes but that they’re still staying lazy?! I would love to come consult with you but I live in the UK!
Thanks so much.
Hi Nicole. Great to hear from you…all the way in the UK! It sounds like you are doing diligent work on your side glute (glute mediues), but missing an exercise to target the back glute (glute max). That is really the main guy to get firing to have more significant relief. Try fire hydrants, have your Pilates Instructors teach you the glute lift on the Tower (push-through bar..they should know) to get a good sense of that glute max. Honestly, it can take 6-9 months or so to really dial down the piriformis hypertrophy and activate the good stuff. And, yes, sitting is a big aggravator. Seriously, stay hopeful. I treated someone recently who had your same issue. It took her a bit to find the glute max, but once she did, she noticed it easing up quite a bit. Thank you so much for your comment. Please reach out if you have any more questions. Lori
Lori, I just had a good deep tissue massage yesterday and at the conclusion of the treatment,f the massage therapist told me that my piriformis muscles are both tight and are causing my hips to rotate outward. I am a 52-year-old male, very fit and a former cyclist. I used to log 7000-8000 miles a year in the saddle. I abandoned the activity about 7 years ago and have replaced it with strength training 3 days a week and cardio 2 days a week. I was diagnosed with severe osteoarthritis of the right hip joint two years ago. I saw a sports medicine ortho who specializes in hip repairs and replacements upon initial diagnosis. After looking over the MRI study of my hip, he said the arthritis was too far advanced for any surgical treatment other than a complete hip replacement and he sent me back to the ortho to whom I had originally been referred. After reviewing the outcome of my visit with the sports medicine doc, the ortho doc suggested that I do my best to manage the pain for as long as possible to avoid a hip replacement procedure for as many years as possible. It was suggested that given my level of fitness and activity that I would wear out a replacement quickly and I would end up needing multiple replacements over the course of the preceding years. At the time I had taken up running on a treadmill as my primary cardio exercise and the doc strongly urged me to switch back to cycling as better way to get my cardio exercise and to limit any activity that was high impact. I did try some stationary bike and I even dug my bike out of storage and did a few outdoor rides but I found that it aggravated my hip pain. I have since settled into training on the eliptical machine and find that it doesn’t cause my hip undue stress. After the comment by the massage therapist yesterday she also suggested that much of my hip issues could stem from the tightness of my piriformis muscles and the way that they are rotating my hips outward. I have no pain in my left hip and have never noticed tightness in area of the piriformis. I have noticed for a long time (probably 10 years or more) that my right foot mtends to rotate outward when I lay down. I always thought that was just the way I was constructed. This has been a longer than intended route to get to the root of my question, “Is there value in seeking PT for my piriformis tightness and hip issues?” The orthopaedic docs did not suggest any and only suggested that I keep on with my daily workouts but limit all activities that cause pain in the hip. I know that there is no miracle cure for the arthritis but if I can strengthen the musculature that supports the joint or decrease inflammation somehow I would definitely seek out help.
Hi Mike. Thanks for your comment. A few things to consider. The piriformis muscle is only an issue when the gluteus max (and to a lesser extent the medius/min) are not working correctly or at all. That is why cycling was likely bothersome because one of the main power producers on the bike is the glute max. But, if it doesn’t work, that piriformis will kick in and do the work. And, that leads to the dysfunction you’re feeling. So, yes, PT would be helpful for someone to teach you the correct neuromuscular firing at your hip. Second, have you considered looking into hip resurfacing? That can be a very viable option for younger, active athletes with early arthritis. I’m not sure where you live, but in Colorado Dr. James Rector is well known for this. Please reach out to me via email with further questions. [email protected]
Hi Lori
I am a 48 year old guy who strength trains 4 times per week. I have a historical L5/S1 disc sequestration that rarely bothers me now. I squat and DL with no issues most of the time.
Mobility is not great and I have to raise heels to squat past parallel.
Last week I squatted after a 2 week break and probably overdid things – net effect was very sore quads and glutes the following day. My glutes however became much worse and ached deeply, accompanied by some sciatic pain down my left leg (reminding me of what it felt like 9 years ago when I ruptured my disc)
I am fairly sure there is no back injury this time – when I roll my glutes and psoas it seems to help so I feel there is a link between very tight quads and psoas and my glute pain.
I have two questions – first of all what is the best plan to reduce the acute pain (I am comfortable only sitting but struggle to walk or to lie flat)
Secondly what would you recommend to address this problem longer term apart from better warm up and mobilisation?
Many thanks in advance.
Peter
Hi Peter. Acute pain is best relieved with ice. It works and is really cheap. Also, I would gently try to stretch in planes that feel good, but not too intense. Second, you may want to visit a local PT and see if your glutes are really firing or if you are using some of the smaller ones (ie. piriformis). A good PT can figure this out really quickly. In the meantime, I always recommend clams (side glute) and fire hydrants or glute lift on elbows (back glute). I tell all my endurance athletes, lifters to do these and some other core/glute firing BEFORE the workout to wake up the neuromuscular connection. This ensures the correct muscles fire. And, yes, tight quads and hip flexors (psoas) will inhibit the strength of the glutes! I hope that is helpful.
Hey Lori,
My partner is one of the unfortunate ones who’ve had their Piriformis Calcify, how effective are the exercises at helping relieve the pain in such circumstances, what things have you heard that will help in this situation, any links you can provide?
Thanks
Hi Ryan,
Thanks for your question. I would definitely give a “go” at training the good glutes to see if that relieves the piriformis syndrome pain. How do you know it calcified? MRI? Ultrasound? Just curious. Botulinum toxin could give relief, but research shows it causes atrophy and fatty infiltration of the muscle. I would rather decrease the tone of the piriformis by non-use (so use of the good glutes) than make it fatty and weak. Pilates side series is a GREAT way to train the glutes. Do you have Pilates Mat classes or Reformer in your area?
Most of the Pilates classes are out of the area, They did an MRI after an accident and then leaving it untreated for way too long (possibly a year?), Unfortunately the only Pilates in the area the instructor treats it more like a dance class than a Pilates class.
Hi again. Well that is too bad about Pilates. Here is a link to a few top glute exercises I prescribe. I am in the process of filming some Pilates videos, but it will be a few months. I would say this, give glute and core exercises a good go. It’s better than nothing!
Glute exercises
I have been suffering for two years now, Ive given up on the massage therapy and physio as im not insured and felt it a waste of money. Sitting on a tennis balls is so painful the pain goes from 9/10 to 200/200. I did yoga for two month everyday for 90 minutes and still no relief. My last Marathon at mile 7 I was crying in so much pain and finished in 4 hrs (not the sub 3.30 I was expecting), I have Boston and London in a few weeks and the pain at the moment is so bad Im finding it difficult to sleep. Running at a slower pace does help control the pain to some extent or at least allows me to run longer but I know deep down running a marathon is going to cause some pain at some point through the 26 miles
Can you suggest anything to do over the next 3 weeks to help? and just curious but do you think wrong running trainers may be a problem? I over pronate and was fitted for running trainers at my local running store which 2 years ago was the best thing I did but I have always purchased the same trainers since?
HI Sue,
Two years is a long time to deal with this. Do you truly think it is just piriformis syndrome and not coming from your spine? Have you had an MRI? Do you strength train your glutes? (Squats don’t count 🙂 ) To answer your question: shoes can be a huge issue. Not always, but they can be. I think we make a big deal about pronation/supination and sometimes we try to mess too much with a person’s natural anatomy. That said, if you can have someone take a video of you running from all angles (maybe a treadmill run for a few minutes), I may be able to give some insight.
In the meantime, ice is the best for pain. If the nerve is really inflamed, a Medrol pack (tapered prednisone pack over 6 days) can be helpful to decrease inflammation and pain. But, only your MD, DO, PAC-C or nurse can prescribe that. If you haven’t tried that, it may be a way to “get through” your race.
Please feel free to send a short video link to [email protected]. OR, a faster option. I do evaluate/consult via video if you would like me to watch you run, analyze muscle and motor firing patterns. Let me know!
Hi thanks for really incitedul article and responses. I have just had MRI that says I have atrophy of right piriformis not hypatrophy is there a difference in treatment, apologies if this is a stupid question
Hi Simon. That is not a stupid question at all. Atrophy is non-use of the muscle and it becomes small with decreased tone to the muscle. A normal level of tone in the piriformis is important so it can act like a sling for the sciatic nerve. Yes, the treatment would be a little different. Are you seeing a PT in your area? They should incorporate some internal and external rotation of the hip to affect all aspects of the piriformis muscle. Very interesting that it’s atrophy and not hypertrophy. Hope your healing goes well. 🙂
I was wondering if there is a connection between piriformis syndrome and pain on the outside of the shin just below the knee? I am dealing with a combination of piriformis syndrome and IT band syndrome and my main points of pain are the left glute and the outside of my left shin. I used to have severe pain on my lateral knee (the IT band diagnosis) but that has gone away after months of PT but the glute and shin pain still is lingering?
Is this likely to address the issue if it was caused by a trauma? I fell over a year ago against the edge of a plank that caused a bruise across my piriformis and caused a minor fracture in my cocccyx, which had already healed by the time an MRI was done. I didn’t see a doctor about this until almost a year after the incident after the sciatic pain wouldn’t go away. I have now been seeing a chiropractor, who said the sciatica had nothing to do with the trauma, but rather was caused by compressed discs in my back, but she hasn’t hasn’t really helped. My primary care doctor and orthopedist didn’t really seem concerned and had no suggestions to help, even though this started with the trauma. I run as well as do yoga, pilates, and strength training but the pain just won’t go away. Of course, running aggravates it but I don’t want to stop that unless absolutely necessary. Should I be getting other tests done?
Hi Maria. First, sorry about your fall. That sounds painful. Well, something is clearly keeping your sciatic nerve not happy. Have you had an MRI on your back (not hips for the piriformis) to rule out if something in your back (disc, osteophyte) is touching one of the roots of the sciatic nerve (usually L4-S3).Sciatica is either from the spine or piriformis. It really could be from that traumatized piriformis from your fall. Have you had any manual therapy work on the insertions of the piriformis or even gently across the muscle? If that muscle was torn from the fall (ie. bruising) then it may have healed with some thickened tissue or adhesions. And, I am curious if you are actually firing your true glutes or just “hanging” on muscle fibers trying to do some work. Where are you?? Maybe I can recommend someone in your area. Or, I do offer video consults and treatments for those of you needing some fresh eyes. I am able to see and diagnose faulty movements and muscle activation. Hope some of these suggestions help.
I’ve had an MRI and an x-ray that showed mild degenerative disc disorder consistent with my age. Two discs are somewhat compressed. The chiropractor was just doing spinal adjustments and doing the massage/digging into the muscle you talked about in the article with suggestions for stretching and strength training that were not challenging for me so I doubted were addressing the issue. I am in Washington, DC so if you could recommend someone in this area, that would be great!
Hi again Maria. Yes, I think you need to another set of eyes looking at your movement and symptoms. I asked my PT colleagues about people in DC 🙂 I was told the outpatient PT clinic at Georgetown is great and Holly Kreisle, PT (another clinic) is also wonderful. Hope that helps!! Please reach out if you have any other questions/concerns.
Great, thank you!
Hi Lori,
I stumbled across your site while looking for info on how to deal with piriformis syndrome, which my doctor says I have. This problem has been going on since February and just getting worse and worse. I think it got worse because I didn’t know what it was at first — just thought I strained my right hamstring. Finally went to the doctor last month. She prescribed physical therapy, which I haven’t gone to yet due to issues with my insurance. The primary pain (quite severe) is in the back of my right upper leg. Lately I’ve been having trouble standing upright. If I bend over to pick something up, then my leg spasms horribly, and I’m unable to stand up straight again. What I have to do is sit down for about 15 minutes, and then I can stand up straight again. This seems odd to me considering sitting is painful (in the right butt area). Any advice on what I can do to regain the ability to stand up straight? Is there something more going on than piriformis syndrome? Maybe psoas syndrome? Thanks for any help!
Hi,
I’m not convinced you just have piriformis syndrome. Although it is annoying condition, in general, it doesn’t make us not want to bend over or stand upright. I am unable to diagnose without seeing someone, but your symptoms make me think of a disc herniation more than piriformis syndrome. And, yes, you can have a disc problem without having any back pain, just leg pain. If you’ve had this since February, you may want to consider an image to rule out any spinal contribution. Your function (sit to stand) is now being affected and that’s important to address quickly. And, if you need to pay for PT out of pocket…do! Being out of pain is worth the time and money.
Hi,
Thanks for taking the time to reply!
Hi, my husband has been suffering since last year (november, december), his problem is spasms down the left leg starting in the buttocks, his moves into his rectum area giving him the feeling that he has a tennis ball lodged in there, it is very uncomfortable, after every bowel test known it is all clear and not a bowel problem, the latest dr has diagnosed piriformis syndrome, he does sometimes get relief from rolling on a ball or exercise roller but the pressure that mounts is so uncomfortable he doesn’t sleep because of it. I have read all the comments above and no one seems to be mentioning the buttocks pressure, would be interested to hear your comments on this being a part of piriformis. He has been told to do kinetics physiology which he starts next week, after 8 months tho I am afraid he isn’t too confident.
Hi Linda. Has your husband had an MRI of his lumbar spine? It sounds like they have cleared the bowel itself, but there are nerves from our lumbar area that affect the bowel and bladder. It is not a common symptom of piriformis syndrome and I would encourage your husband to ensure all is ok with his lumbar spine.
Thanks so much for responding, unfortunately the dr we are seeing doesn’t seem to think there is much wrong and wont really listen to our ideas, I would love to get an MRI but don’t know how to go about getting one. Long story short we left our dr for more help now wish we didn’t, might have to swallow our pride and go back with our tails between our legs ha ha. He is seeing a chiropractor who thinks he can help but said it will take a while (we trust him from previous visits), I like the MRI idea, will work on it, the kinetics psyiology which he starts next week hopefully will help. Thanks again, we are getting desperate!!
Where are you located? I would be determined to clear that lumbar spine. May be nothing, but it’s worth the effort to find out.
We are in Mildura, Victoria, Australia, have started to make arrangements to go back to original dr, think he will be ok to approve an MRI. The pressure or feeling of a tennis ball being stuck is quite debilitating, not sure why the other dr wouldn’t address it, am really grateful you have taken the time to respond, we have been feeling quite alone on this and now I know that I have to push for the MRI. Thanks so much.
Excellent article! I found that stretching and rolling were making the injury worse. So, I stuck to banded glute bridges and clam shells. It worked wonders and made me stronger. I was even ability to achieve more in my athletic career by addressing it this way. Thanks! Keep up the good work!
Fantastic! Thanks for sharing.
Hello followers of this blog post! For those of you looking for a quick, healthy glute routine, I just made videos!! One for abs, full body and THE GLUTES!! Check out the link:
https://vimeo.com/duncansportspt
Lori, your article is right on the money. I spent 6 years wrestling with PS and learned a lot about what works and what doesn’t. I’ve written a PT protocol for PS which focuses on how to strengthen and re-activate the glutes. This helped me to bring the PS to a more manageable state, but frankly in lengthy chronic cases like mine there may not be full resolution. Piriformis release is a fairly simple procedure which if done by an experienced surgeon can be done on an outpatient basis within the span of an hour or two. If the glutes have been strengthened prior to release surgery, the patient won’t notice any change in hip control or pelvic strength, and can literally be walking the same day and largely recovered within a couple weeks. It’s not really as draconian as you may think, and if it helps, is well worth it.
Hi Jim! Glad you finally have relief from that syndrome. I always say there is a time and place for surgery, but most people think it’s the first place to start. So, you’re right, if you have tried all of the conservative routes and truly activated the glutes, that surgery would be minimal. Most people who get the surgery are just looking for the quick relief and never really solve the issue. Thanks for taking the time to reply and happy it makes sense!
Hi Lori,
Great article! I have suffered flare ups of this for several years. I have been seen by several p.t’s for issue, but it keeps reoccurring. And it seems any attempt I make to exercise the glute max, causes more pain in the hours after I finish the exercises. I seem to be feeling the clam exercise in the right spot. But the fire hydrants on the affected side, I feel more in the oblique??? I watched the video and don’t feel like I’m twisting but it is definitely feels different on the (left) affected side and is causing more pain. Any insight you could provide would be appreciated.Thanks
Hi Eric. Thanks for you comment and question. It sounds like your brain (yes, the brain) is having a really hard time figuring out how to activate your glute max. So, it keeps using the piriformis or now your oblique. Fire hydrants are great if your brain can figure out all three motions at once, but it sounds like we need to break it down for you. You need to start with a “mule kick” in really specific way. Get on your hands and knees, hands under shoulder, knees under hips. Now go onto your forearms. Place a block or stack of books under your “dysfunctional” side so your knee rests on it. Engage your core so your pelvis stays level. From that position, try and lift your leg up in a small range of motion- USING THE GLUTE…not your back or hamstring. It’s a subtle movement, but once you do it right it will start to shake and feel isolate to the back glute. Let me know if you have questions or want me to help you via video…I do offer that and people get better!
Hi Lori
further to my last comment (about a year ago!) I wanted to report that my piriformis issue … which made my life a misery … is GONE!! I have been pain free for about 6 months now. Occasionally if I slack off the pilates for a few days, or do a lot of sitting, I feel a twinge – but then I just get back into good habits and it goes away. I attribute this for the most part to the insights in this post which together with months of daily (often boring!) glute exercises and weekly classes with my regular Pilates instructor have made all the difference. I really think you have the key to solving this awful issue – at least you did in my case. So thank you very, very much!
Best wishes,
Nicola
Hi Nicole! I have to tell you this comment makes me SO happy. Good for you for doing the “boring” and important work to train the right muscles in your body. It is so painful and I’m very happy you are no longer dealing with it. And, thank you for taking the time to write about your experience! This truly warmed my heart. All the best! Lori
Nicole, after discovering Lori’s article and blog I so hope I’ll be able to write like you have, that I’m out of pain. Question for you…what tips do you have for long car rides/trips? I will often take my seat belt off for a few minutes and turn around with my knees in the seat. Have you found anything that works for you?
Lori, I obviously don’t know what I’m doing here. If you have a way to delete those posts please do. I’m reading your whole page today and printing several pages to take with me to PT tomorrow. I’m 3 years in to PS. 🙁 Do you have a “mule kick” video that you talked with Eric about here on 12/10/16 that shows very specifically how to do it correctly?
Hi April,
I have a glute Pilates video (15 minutes) that you can purchase (cheap!) and I show how to do it in that. Click above on the website where it says “Pilates on Demand” and it will take you to the Vimeo site. Hope that helps!
Nicole, after discovering Lori’s article and blog I so hope I’ll be able to write like you have, that I’m out of pain. Question for you…what tips do you have for long car rides/trips? I will often take my seat belt off for a few minutes and turn around with my knees in the seat. Have you found anything that works for you?
Hi. I’m an Englishman of 64 living in France I’ve been suffering from Piriformis syndrome for about a month. It started after too much work with the chainsaw. Then a long drive over several days. I’ve seen my doctor, osteopath, chiropractor and, here in France, a kinésithérapist. The problem is that the pains are always worse after treatments, especially with the kines. The best it’s been is since I found your site and started working on glute strengthening exercises. Almost ignoring the piriformis itself. I thought it was getting better until a recent kine appointment when he used a TENS machine on the muscle. There followed a horrendous night. Up every 2 hours or so needing to walk around until the leg pain subsided. My inclination is to stop treatments and concentrate on your regime of glute strengthening exercises. Or should I seek further advice elsewhere. Thanking you in advance.
Hi Paul. Thanks so much for reading and reaching out. Yes, I think your instinct is right to stop treatments for now and try to find your glutes. It sounds like the TENS somehow activated the muscle, irritating the sciatic nerve, thus your night of pain. My advice would be to work on finding the glutes for 4-6 weeks and see what happens with your pain. Please reach out with any other questions or to check back in a few weeks. Happy Glute Finding!
Thanks so much Lori for your prompt response. 3 days since the TENS session and i have continued religiously with the glute exercises. I’m doing the last ones just before getting into bed. Last night was the best I’ve had in weeks. I’m hoping to get back to some regular walking too and have determined to not allow anyone to aggravate the piriformis again . It would seem this approach of taking the load from it and letting it heal is the solution. I’ll certainly report back on my progress in the New Year. Hoping my experience may also be of interest to fellow sufferers.
i just came across this article. I am a triathlete that has had about 4 years of hip/SI joint/piriformis pain. I had done chiropractic, and PT. I have glut atrophy on the right side. This is as concerning to me as the pain. I have been doing clam exercises etc, but still have atrophy and still have bouts of sciatic symptoms, especially if I do much exercising. I have quit running completely. Did biking over the summer along with swimming, but still have problems on and off. My question is will the atrophy ever get better>?
Hi Christy! Thank you for your comment. Short answer, yes, atrophy improves as long as the neuromuscular connection exists. What do I mean? The inferior gluteal nerve supplies the glute max and the superior gluteal nerve supples the glute med/min. So, as long as no one has been in there to cut that nerve and that nerve is healthy, then YES! Atrophy is just a state of the muscle not being used. It sounds like you are still having a hard time with activating the true glutes instead of the piriformis. Since it’s been so long…has someone cleared your spine? Just to make sure you’re not getting any pain from that level? If the spine has been cleared and it is just the piriformis, make sure you are adding in a glute max (back butt) exercise. Fire hydrants work well. Please reach out with any further questions and thanks for reading.
Hi Lori, I am looking for some advice, I have been suffering for 4 weeks now with deep buttock pain which radiates down the back of my leg (left), it started a few weeks ago when I had trouble getting out of bed and walking, the pain is quite bad, I have trouble sitting for any length of time and also bending and cannot lie on that side. It is generally eased by walking. I have been to see a physio (privately)and he has diagnosed Piriformis syndrome and has given me some stretching exercises to do at home which I have been doing daily along with some massage using a ball. I am based in the UK and have also seen a physio on the NHS for some more help and he has told me that I don’t have PS but a muscle weakness in that area. I have a history of right sided abdominal pain and have had 4 surgeries in the space of 2 years last surgery April 16 for adhesion removal, in view of this I have weak abdominal muscles. The physio who diagnosed PS has said that on palpation of the piriformis muscle it is markedly tender and stretching of this muscle is also tight. I also have spondylolisthesis grade 1 which was diagnosed in 2013 after a routine x-ray and advised that I was probably born with this condition, I have no back pain or other issues from this. I have private health cover but it excludes anything related to my spine/sciatica and I have been in touch with them for help but are being somewhat unhelpful, the physio does not think that my problem is any way related to my spine either. I have been advised by the second physio to not do any stretching exercises but strenghtening ones, basically all the ones that I was advised to do initially. I have been given an exercise to do, standing up though which I feel over the past few days has made my condition worse, and I have more pain and have had more disturbed sleep and have been awake in the early hours. I have a pilates reformer and I am happy to use it, but need the right advice and exercises to do. I am beginning to think that the first physio I saw knew what he was talking about and had the correct diagnosis, he has many years experience and has worked with professional footballers and seemed very knowledgeable. The second physio did not seem that knowledgeable to me and was a lot younger and obviously a lot more experienced. I would be grateful for any information or advice that you can offer me. Many thanks.
Hi Sue,
Thanks for reaching out. That is a big history and you likely have multiple things going on. However, strengthening the deep abdominals and good glutes is essential for almost any diagnosis. That said, I have posted the top 2 glutes I use in the clinic and they work with time. I would stop stretching the area and possible doing any exercises that aggravate your symptoms. As for Pilates, YES! It sounds like you may need to take some private Pilates sessions where you are (maybe 4-6, spaced out every other week so they can show some specific exercises). Unfortunately, that is challenging to prescribe Reformer exercises via the internet. Ask the pilates instructor to show you deep abdominal work in various positions, side series (glutes) and stomach massage series (this is very helpful for hip range of motion and lifting out of the pelvis). Hope you get some relief soon and thanks for reading!
Hi Lori, thanks for your response it is much appreciated. I have seen my Dr and have an appointment next week with my physio, I need to explore getting an appointment with a consultant and having some further tests/scans etc, in view of my previous history. I will look into some pilates sessions also. Kind Regards, Sue
I have a connective tissue disease (scleroderma) and have been struggling with this for many years. Every time I do much of anything I get a new injury with accompanying inflamtion. By increasing the load on the GMax and GMed will it most likely take longer for my piriformis to heal from the hyperteophy since I have a CTD? I just feel like giving up ? I do also have some disc herniation in L-4/L-5 and L-5/S-1
Hi Angela,
Good question. I’ll be honest, I’m not sure. Even without scleroderma, piriformis syndrome can take MONTHS to relieve. But, I wouldn’t give up. If this is new (finding your good glutes) please try it! As you can see from the thread of comments, with time and the right exercises, it will go away. Are you under the care of a physical therapist? And, are you sure your piriformis pain is not coming from your spine?
Dear Lori
Your article on piriformis makes sense. I’ve had problems with my lower back since I was in my late 20s and at around the age of 37 I underwent a spinal fusion and decompression S 1 L 5. – the pain reduced but never left me. I’m now 64 and as of late I’ve been having more piriformis problems. I have deep massage each week. – sometime I get a few days pain free. So walking for twenty minutes, sometimes less produces the pain as does standing – almost instant. Sitting doesn’t help! But I can get up and move around. I stretch every morning and night and I used a recumbent exercise cycle two to threee times a week for 20 minutes. Only the tennis ball or massage gives any relieve at all but as you say – not good therapy.
Could I arrange a skyoemsession with you?
Many thanks
Ian
Hi Ian,
Glad it makes sense! Yes, please contact me at [email protected] so we can arrange a time to help you figure this out. Look forward to hearing from you!
This is a great article. I am a pediatric physical therapist and I have piriformis syndroms. Every problem I come up with as I train is usually from weak glute meds, but for some reason I just never believe it until I have an out-patient PT test my strength and remind me “you’re only a 4-/5.” This makes absolute sense. Thank you!
Hi Erika,
Thanks for reading and the reply. I’m glad it makes sense to another PT!
Hi Lori,
Thank you so much for this article. I am a writer in my 50s who has been suffering from piriformis pain for 8 years now. I had to stop physiotherapy because the exercises were making the pain worse. Recently, I started trying the exercises I was giving (stretching plus clamshell, bridge and side leg lifts) but again, it is causing more pain. I am desperate to avoid surgery but don’t know what else to do.
Any advice is appreciated.
Hi,
8 years?? Oh that is so long. I would stick with clamshells (make sure you control that pelvic rotation) and fire hydrants. These are non-weight bearing (feet not on ground) and allow our brain to figure out how to find the good glutes. Bridging is more difficult than we think and we can compensate with all sorts of muscles (quads, hamstring, piriformis).Stretching is not great for this condition. It usually exacerbates the problem. You are clearly not a surgical candidate from the MRI results, so don’t go there. We all think surgery is the “quick fix” but it is not. And, your MRI shows nothing to fix (at least per your report). It sounds like a muscle patterning problem that needs attention…stay encouraged!
The problem is that even clamshells make the pain considerably worse. Sometimes so much that working the next day is impossible without large doses of pain killers. I don’t know if I am doing something wrong. But ANY exercise that uses the glutes or hip flexors makes the pain far worse. I am in despair over this.
Re: MRI. I gather from talking to other doctors and sufferers that the standard MRI will not always show piriformis syndrome. Is this incorrect?
Hi Mariekel,
When clams make the symptoms worse, stop doing them! They shouldn’t. So, either the form is not correct OR your brain simply can not figure out how to find the good glutes without recruiting the piriformis. It’s rare, but it still happens. It’s why I say they are the “top 2 I use in the clinic” not the “the only 2.” MRI will not show piriformis syndrome, only that the piriformis has hypertrophy (thickeness). However, an MRI will diagnose a spine contribution (ie. disc, stenosis, etc). I do not advocate getting an MRI unless needed, so if you think something more is going on, you may want to consider it. Piriformis syndrome WILL heal itself with the right glute recruitment…you just have to find the right exercises for you.
I should mention that i have had MRIs (they show nothing, not even inflammation in the piriformis area) and x-rays of my spine (everything ok as of a year ago except mild arthritis in the base of my neck).
My experience is similar — neither MRIs nor an MRN showed anything. I was diagnosed with PS with a provocative EMG. I also find clamshells cause problems, however there are a few exercises focussing on glutes (single leg glute bridge and another form which recruits additional rotators) which have helped a great deal. I also do a couple yoga stretches – trikonasana and another variation which have been very helpful.
Hi Jim,
That’s interesting that single leg bridges work for you, but GREAT! Pilates side series is also another great exercise series I use. Trikonasana- yes, that can be an excellent feed into the glute med/min. As I told Mariekel, it’s about finding the glute exercises that feel good, not bad. Clams and fire hydrants just happen to be the best for MOST people…not everyone. I also love Pilates side series and if you put your leg into a theraband while doing it…can be magic!
I understand and have done most of those. The exercises that work for an individual certainly vary depending on where the compression of the sciatic nerve occurs along the piriformis. There are actually two areas where the sciatic nerve can become compressed — 1) where it passes the piriformis (typical), and also 2) close to the spine where the piriformis attaches to the sacrum — the sciatic nerve passes under the piriformis at this point as it emerges from the base of the spine near the sacrospinous ligament, so it is still not spinal sciatica, but also not ‘mid-butt’ like many. This is a much tougher form of PS to address.
Jim, could you please share the specifics of the exercises that have helped you? Even a few clamshells exacerbate the pain for me. Many thanks.
Mariekel, I don’t want to distract from Lori Duncan’s excellent guidance here on her blog (she is our host, thank you again Lori). I have over the past seven years seen 7 or 8 different PTs, and ironically there are now 2 members of my immediate family in graduate programs for PT. I have also had PS release, so as they say ‘been there, done that’. Good news is that I’m feeling better, little by little, and still hoping for full resolution. Bad news is I haven’t found a single 100% ‘cure’ but rather a hundred 1% cures… I’ve written a couple page overview of what has helped me which is emailable (but not assoc’d with Lori’s blog or practice), so it’s not something I can share here. BRGDS/JIM
Is your write up available online anywhere? also, you said you had piriformis release surgery, if I understand correctly? what was your experience with that, including time off work and recovery generally? I am rather desperate for help.
Hi again Jim,
Everyone thinks there is this miracle “cure” with elbow treatments and stretching. PS is a NM patterning problem. I’m treating someone right now who’s issue is that he didn’t rotate correctly. It was a patterning problem. Got him to rotate in correct order, which then allowed his brain to organize and find the correct muscles. I’m sorry you have had pain so long, but in my clinical experience, it has always been treatable.
Mariekel,
No it’s not online and as I mentioned, I don’t want to distract from Lori’s excellent advice. If you want to discuss privately, feel free to contact me at [email protected] RGDS/JIM
This is the first potentially helpful thing I’ve read about treating piriformis syndrome. It makes total sense in my case that the glutes have been underworked and the piriformis overworked. I know just how my ps evolved, so I will try your glute therapy to see if that helps. I suspect it will, since walking on flat sand on the beach where I live aggravates the piriformis/sciatic nerve, but steep uphill hikes where the load is transferred more to the glutes feel fine.
Any additional exercises I can do on a Pilates reformer? I happen to have one, although I confess it’s underutilized at present. Are there exercises I should *not* do until my ps is healed? Many of the legs-in-straps movements stretch the piriformis.
Also, is there any palliative care I can take while I build up the glutes? My pain is worst in the morning for a few hours until I get going, and it seems like no matter what position I sleep in, I wake up in pain. Some days are worse than others, and it’s totally unpredictable. I can’t lie in bed for more than about seven hours, but I really need eight or nine hours of sleep. The only pain med that seems to touch it is tramadol, and in addition to tolerance issues, I don’t like the potential for addiction. I’ve tried naproxen, acetaminophen, heat balms, etc. Heat? Ice? I live in a Latin American country with few knowledgeable medical resources in my area. This pain is no longer a nuisance and really starting to affect my life.
As a former professional dancer with a subsequent background in clinical healthcare delivery, I can really appreciate your site. Thank you!
Hi Patricia,
I’m so glad you made a response. Yes, get on the long box, on hands and knees, one foot in strap (easy spring) and lengthen the leg behind you. Like a modified bird dog. That exercise makes you use the correct glutes and stabilizers or else you just fall off the machine. I’m not sure of your skill on the Reformer, but squat and single leg squats are also good. If you’re in the wrong muscle group, it doesn’t go very well. 🙂 Hope that helps and keep me posted on your progress. And, try the clams and fire hydrants…miracle workers if you do them right.
Thanks, Lori! I will try the exercise you suggested, in addition to the clams and fire hydrants. I try to stay away from squats because of knee problems. I feel like if I were to do them wrong due to lack of strength/balance, I’d wind up doing a big face plant on the front of my machine. It’s something I might be able to work up to though (at least with both legs). Maybe I can try them with a friend to spot me just in case.
Lori,
Do you have any suggestions for what to do about the pain while sitting? As i mentioned, i am a writer and am frequently in pain. Every doctor and physio i have seen says stretching is what to do for the pain, but that has certainly not helped. I cannot keep taking high does of ibuprofen.
Many thanks.
Hi Mariekel,
Yes, stretching is very aggravating for this diagnosis. So, stop that now. 🙂 Do you have the option of writing while standing. Our bodies were not meant to sit, so if you can stand that will likely relieve some pain. If clams are bothering you, try a sidelying straight leg raise. Go to a wall, put your back, pelvis, heels along wall (keep heel on wall for support). Lift leg up/down to feel the side glute. If you must sit, sit on ice.
Do not have the option to stand, alas. Ice does not seem to help much, but perhaps I am not icing correctly. how long should I apply it?
Maiekel, I also work as a writer and spend a lot of time sitting. I don’t have great knees, so standing for long periods doesn’t work for me (and my workspace isn’t really configured for that either). One thing that has helped me when my butt starts to get sore while working is to place an ottoman under my desk. Then, I can at least sit with my legs extended, which allows me to stretch my hamstrings. It also lets me lean back a bit, which makes my hip flexion less acute.
I try to get up every hour or so to walk around, do a little housework (I work from home), or get a glass of water, although it often winds up being more like two hours between breaks because I don’t want to disturb my sleeping dogs or my own concentration. To remind me to take a break, I use the Pomodoro app on my laptop; it can be set for any length of work/break time and chimes when it’s time to stop/restart. I hope that helps. I literally feel your pain!
HI Lori,
Thanks so much for this article and for all of your replies; it has all been very insightful. My husband has been suffering from what we think is mainly a piriformis problem. I have two questions:
You mentioned that “just” stretching will likely not help the issue, but do you think that it would help in conjunction with strengthening weak muscles? Or should we lay off stretching all together? We’ve been doing an MET piriformis stretch (among some other stretches) twice a day for about a week, and he has noticed some (good) changes in his buttocks/leg pain, such as reduced “tingling” in his lower leg.
Also, my husband does have trouble standing straight, but he doesn’t think that it is a disk issue (he has experienced a disk issue in the past, but he says this is much different. We’ve read up A LOT on PS, disk issues, and innominate dysfunction, and he strongly believes it is his piriformis causing all the pain). When he walks, he hunches over a bit (bending at the waist) in order to relieve the pain that he would otherwise feel standing straight (mind you, he’s only 30 y.o.). I was just wondering if the pain relief from hunching could be that the glute med and glute max are more engaged in that position, thus forcing the piriformis to relax a little? Would this make sense at all?
We will be starting your recommended exercised TODAY! Thank you so much for all of your help 🙂
Kelli
Hi Kelli,
Thanks for reading. I would lay off stretching. It’s usually not a length issue, but a problem in the brain that it uses the piriformis instead of the good glutes. To your question about standing, that could be so many things and difficult to answer in a blog response. I would recommend finding a good physical therapist in your area to address his movement compensations.
Ok, we’re gonna focus on retraining the brain with clams and hydrants for now, and see if that helps. Thanks so much for your advice!
Hi Lori,
Thanks for this article – it makes a lot of sense. After reading it, I think mine may have been triggered by weak glutes and walking ‘crooked’ from a preceding, and occasionally recurring back injury.
Every time this injury would flare up and start to get better, I noticed mild sciatica as it was healing. I thought it was just part of the healing process, but now I think it was my piriformis responding to the crooked walking. Except this time, its bad and won’t go away, and the stretches the PT is making me do does not seem to be helping.
It hurts when I sit, stand too long, or walk too much. Since it hurts when I stand, does that mean I may be standing (and walking) incorrectly and relying too much on the piriformis? And if so, would you advise I correct it?
Thanks again for this article!
Gil
Hi Gil,
Glad it makes sense! Yes, if your brain only knows to use the piriformis, that is all it will use in standing, walking, etc. Yes, correct that! Train those good glutes, stop stretching it and maybe have someone help you with your recurring back pain?! Our body is one continuous unit and it is all related. Thanks for reading and your comment!
Hi Lori,
I just wanted to thank you for this great post! I am a PT who has been experiencing SEVERE glut pain and spasm with radiation to my dorsal foot for weeks. This arose about 2 weeks after a minimally invasive TKA for a degenerated varus knee. I am 52,in decent shape and thought I would whiz thru my rehab but this pain has been completely debilitating to the point of only non weight bearing amb with crutches.I think my entire lumbopelvic balance was thrown off by my new “long” leg after 30+ years of adaption.
I have had a couple of PTs, massage therapists, a DO, and even a chiropractor look at or treat me in addition to a lot of self treatment with little improvement. After switching PTs and reading this post I realized I was making myself worse with aggressive STM to the gluteals and piriformis. Gentle SI and lumbar corrections with ME and MET, combined with a piriformis release with my leg off the edge of the bed on a Swiss Ball and TENS helped calm it down significantly! I have started the strengthening as you describe and am at least 90% better.
I now can get back to increasing the ROM and strength of my knee that has been so limited by the pseudosciatica pain. I have to wonder if I had a traditional TKA and was on a walker for a couple of weeks if my body would have accommodated more gradually?! I’ll never know.
Thanks again for your insightful post. Your patients, and readers, are lucky to have you!
Thank you Lynn for taking the time to write and for your kind words! And, so glad you are feeling better. It’s not enough to have a TKA and then glute pain on top of it! Interesting thought about the walker for B hip/pelvic balance. Sounds like you are on the mend and ready to go help others. I appreciate your response!
Thank you for Shari g this blog. I thought my pain in my butt & hamstrings were just from poor stretching & being overworked (I’m in the army & there is a lot of physical demand put on my legs). I found out from talking to a colleague that my pain might be a pinched sciatic from an inflamed pirifomis. After a year of stretching, not running, & rolling on tennis balls, I could still feel the tightness even though less pressure was on my sciatic.
I’ve started implementing strengthening exercises to identified muscles & can feel a difference after a week. I believe this article has saved me from a lot of pain & possibly prematurely leaving the army. Thank you.
Hi Rebecca,
I’m so glad you are feeling relief. Our bodies are meant to move…we just need to move with the right muscles in the right order. Hope you continue to have relief. Keep up with the strengthening exercises. Thanks for reading!
Hi Lori, I’ve been experiencing symptoms of sciatica off and on for about a year and I’m starting to come to the conclusion through a couple of different health care professionals that my glutes are not firing very well. I’ve concluded that along with my moderate work out plan I’m adding glute specific exercises to help strengthen them. Now my issue is that my sciatica has started to flare up since I started the glutes part. Is this one of the things that gets worse before it gets better?
Hi Jacky,
No, the exercises should calm down the sciatic pain. So, maybe these exercises are not for you. Clams and fire hydrants are top two I find that help people, but not the only two. Others that work for people at times: single leg squats from a high surface so you have to push off from your glutes, laying on your side against a wall and sliding the leg up/down the wall in a small range so the leg feels supported. Just try to find exercises that make you feel glute fatigue, not sciatic pain.
Hi Lori, thanks for writing this great article! I’ve found some information here which I haven’t come across anywhere else. It took me 10 months and finally having a mri to get to a (correct) diagnosis. Some questions:
1) Would you recommend using a foam roller to massage over the area? Or is this a waste of time?
2) What cardio is the safest to do? Some people say don’t run others say run conservatively.
3) Would a coccyx seat cushion be a good idea? There are several that advertise “relief from piriformis syndrome pain”.
Thanks!
Hi Bronwen,
Thanks for reading and your comment. 1) No. Foam rolling is so overrated and used inappropriately. Waste of time and can flare up the area you are trying to calm down. 2)Cardio that doesn’t cause you pain. That can be running (if you can run from your glutes…that is how we should run), elliptical, biking, swimming, hiking (can be great if you push-up from those glutes). 3) Coccyx cushion is a waste of money/time for this condition. I’ve actually never heard of that before, but from an anatomy standpoint, it does not make sense. Find those glutes!!
Hello Lori, I have been suffering with this condition for about a year now, stretching and foam rolling to treat to no avail. I just started with the glute exercises after finding your article. I like to run and bike. My wife thinks the biking actually is the cause of my problem. My question is, do you have any advice on how to make sure we use the glutes when running and biking? I have stopped the running and biking for fear that I am worsening the condition, but want to start them again and do them properly. Thanks for your help! Bill
Hi Bill,
Once you feel like you have found the glutes, then get on the bike. Mod load and start feeling the glutes kick on during press down and pull back (it’s not a pull up stroke). The glutes are highly active at the time. For running, think of yourself propeling from the glutes, not the foot.
This is the closest thing I have found to address my issues. My worst pain is when I get up in the morning. I feel like I don’t sleep well, due to pain, and it’s hard for me to lift my hips to turnover. Then just getting on my feet flares up the pain. Some mornings I just cry while I ice it. It takes about 20 minutes of being upright for everything to calm down. What would the association be to sleeping? THANKS SO MUCH FOR THIS FORUM
Hi Amanda,
That is common that the morning is the worst time and that movement helps. We are meant to move. To your question, sleeping allows our body to relax and from a relaxed state your piriformis (or it sounds like) may be the first muscle to try and move your leg. So, work on finding your good glutes and in a few weeks you should feel better, not perfect, but better. And, as always, make sure you you have had your spine cleared for any contribution to symptoms. Thanks for reading and hope you feel better soon!
thank you….am trying the clam and fire hydrant 🙂
Hi Amanda,
Hope you get relief soon!
Hi Lori,
Wow, I just stumbled upon this article and I am so impressed that you are still responding to comments a couple years later! Figured I’d throw my hat in the ring…….
I have had my issues since February; started as a pinching feeling near hamstring insertion on my right leg so I originally thought it was a hamstring injury. Ended up being diagnosed with piriformis syndrome and went to first round of PT in mid-March through beginning of April. I saw major improvements and wanted to get back to Barre (I had been consistently going 2-4 times a week since June of last year but stopped going when this started) but my husband and I were taking a trip to Hawaii the first of May so I didn’t want to re-injure/recur anything. My issues seemed to have gone away so when we got home I went back to barre and in one day it was all back. Went to one ortho who wasn’t interested in helping me figure out the problem, so I changed to another ortho who got clean x-rays, clean MRI (he was thinking it was hamstring oriented as well), and ended up diagnosed me with “Lower Quadrant Dysfunction” and sent me to a different PT for another round. This PT has not diagnosed me with piriformis syndrome but is working on reversing some central sensitization he thinks I have but he also does manual therapy and adjustments each time after my workouts (I’ve been to 4 sessions) only on my hip and mostly specifically on my piriformis that is in a completely spastic state, guarding heavily (which was also the case in my first round of therapy). I also have a home program I am doing 5 times a week that includes fire hydrants that you have talked about, a couple of stretches, bridges on the Swiss ball and a couple other hip exercises. Only other symptom I have sometimes is discomfort around the SI joint. I do feel like I am making progress, definitely, but I guess I’m just worried about what happens when I get done with physical therapy THIS time, especially since I was feeling almost 100% after my last go and then as soon as I went back to my preferred activity, Barre, it came back. This has been an extremely challenging 6 months for me as I’ve never dealt with anything quite so stubborn/vague. My suspicion is a form problem in barre and very likely the glutes issues that you have mentioned, so how do I make sure that I’m good to go and how do I even know when/if I can return? Any of your thoughts on this are greatly, greatly appreciated. I just want to do everything I can to heal from this once and for all! Thank you so much.
Hi Allie. Barre is cued many ways, so make sure you are using neutral pelvis (unless you are in a deep wide plie) and not the posterior tilt or “tuck” they often cue. It is not correct mechanics for the body. We should be in neutral spine. Some Barre classes are good with that, some not. Make sure you do a set of good glute exercises everyday for 1 month and then every other day after your discharged from PT. Sounds like your body has some old habits and likes to use the wrong muscles. Hope you continue to get relief.
Hi, Lori. Just came across this article and it makes sense. All signs point to piriformis for me (with old, previous Sciatica never issues in the past).
However, looking over diagrams of the glute area, I still feel like every once in a while when I would stand up after stretching a “pop” would occur that felt like a muscle or tendon right along the inside of my butt cheek. Literally, right along the cheek to the tailbone. Maybe 1/8 – 1/4 inch in to my left side. The piriformis pain I feel is about another half inch to the left deep in the buttocks.
Is there something I’m missing? Could I have torn my glute?
Hi Lori! Just been trolling the net & So glad I found your posts on glutes & pirifirmis! Have had left sore weak buttox/hip issues for 15 yrs! First tried massage then pt with therapists. Very tight tfl. Then Chrio. & said I have anterior tipped pelvis. More therapy AND multiple injections over the years. FINALLY After NO Relief I found a ortho. surgeon that “knew” my problem & could “fix” it! Wow! Yea! Something to help! Pirifirmis release surgery:( I now look back and think WHY did I do it but it is what it is. I now over the past 9 yrs am worse than b4. I feel like I am sitting on rocks & can NOT Sit mire than 3 minutes! My MRI says my left pirifirmis is atrophied! I can BARELY bend over due to CHRINIC TIGHT hammies lower back muscles just pulling tight and Constant tight neck & shoulder muscles! Needless to say you know what kind of person this ALL turns me into. I have been trying your 2 clam and hydrant exercise. My legs barely make it up 6inches on clams I am SO Weak. Do you have any suggestions or anyone in the Cleveland Ohio area you would suggest! REALLY REALLY at the end of my rope :(. Thank You
Hi Candy,
Wow, what a journey! I will reach out to my professional base and see if anyone is in that area. Stay tuned…
Than you SO MUCH! Like I say I have tried it ALL. P/T. Water ther. Rolfing accupunture prolotherapy muscle activation act. Release & whatever else is out there. Done it. Been there! As Soon as I do almost Any exercise or just “normal life activities” my body is totally out of alignment:(. and right back to Chrio for adjustment that will not hold! I look forward to any info. you can Help me with 🙂 Thanks!
Hi Lori,
I just saw a rheumatologist today in an effort to treat my left sacroiliac joint pain. All pain is on the left and it often goes down to my knee. On palpation, he said my pain was directly over my piriformis, which actually had a little knot on it. Do you find that SI pain is often associated with the piriformis? My left SI joint is pretty arthritic and there has been some talk of it being possibly hyper mobile. Is this all related? I do totally see your point that the glutes are lazy. If exercising them will fix all of this, I am all for it. I had dry needling done a few times several months ago at PT, but I can’t see how that is a manageable option long term.
Hi Lisa,
Our body is one connection, so everything is related. Piriformis syndrome truly comes from poor glute activation. So, yes, finding good glute exercises for you is KEY! Dry needling can help with pain relief short-term, but good neuromuscular patterns and movement are the only way to truly heal the body. Without movement, all of the passive treatments are not worth anything. Find a PT who specializes in Pilates.
Hi Lori!
I came across your article while doing some research for a patient I evaluated yesterday who was diagnosed with OA at his hips (mild) and bursitis bilaterally. On evaluation, I immediately noted his glute max and med atrophy, while his gastroc/soleous and quads were very well developed. He also presents with compensatory forefoot pronation bilaterally which is quite significant. On palpation, he had no pain at his greater trochanters, but when I got to his piriformis, bingo! He confirmed that was the site of his pain symptoms. He is a tennis player and instructor and his pain has been mostly post play, but he reports that this week, he had to leave the court mid-play, the pain was so severe.
I did explain to him that he was most likely overusing his piriformis to compensate for his glute weakness as you had stated in your blog post. I am wondering, have you noticed a link with forefoot pronation as well and the role of the piriformis in decreasing hip internal rotation acceleration during activities? And if so, have you found that your patients benefited from orthotics in these cases?
Thank you for any insight and if you have any specifics regarding tennis play in particular, I would love to hear it.
I’m so glad I found your blog! I think it will be a great resource for myself and my patients.
Hi Andrea,
I have not noticed that link and have found both pronation and supination. The piriformis pain may limit IR, but once you get good hip on pelvis dissociation, that should flush out. I only prescribe orthotics at the very last moment. Most of us do just fine with the body we are given if we treat what is needed. What specifics about tennis? Happy to brainstorm with you.
Hi Lori
I have had an issue with left buttock pain that radiates into my left leg for a number of years. I always assumed this was originating from my back, but a recent MRI revealed no disc bulges or herniations in my lumbar spine. The only finding was osteoarthritis in the facet joints at L4-L5 and L5-S1. I now think that it may be a piriformis issue as the point of pain is in my left buttock close to my hip with another point of pain near the sacrum with spasms between the 2 points. In the past any episodes of pain usually resolved fairly quick, but currently I’ve had the pain for over 2 weeks. After a week, I took a muscle relaxer and the radiating pain into my leg stopped, but I still have buttock pain and I’m not able to sit or stand for very long. I’ve also noticed that my left foot is pointing outwards most of the time now while standing. My feet have always pointed outwards while sleeping. I have an appointment with an orthopedist, but it is not until November. I’m going to try the exercises you’ve recommended, but I’m thinking it might also be good to try to see a physical therapist. I live in the Folsom/Sacramento, CA area. Do you have any suggestions for physical therapists in this area? Thank you for all the information you provide on your website – it’s very helpful !
Hi Mary,
Yes, OA of the facet joints usually stops around the glute/hip area and does not travel to the leg. But, the longer I treat, the more I realize anything is possible. So, could be spine, could be piriformis. I would definitely recommend trying PT. I don’t know anyone in that area, but look for a PT who is movement-based, not modality (e-stim, ultrasound, etc) based. Good movement patterns are what heals the body! And, someone who truly understands the glute/core complex. Maybe a Pilates/PT combo. And, thank you for reading the blog posts! I’m glad they are helpful.
Thanks Lori ! I really appreciate your getting back to me and for the info on what type of physical therapist to look for.
Hi Lori,
I am (or was) a very athletically fit 30 year old who was recently accepted into the top P.T. Graduate program in the area. Unfortunately, I was forced to withdraw and go on medical leave for the year. Needless to say I was heartbroken.
The reason for my withdrawal was that I was experiencing some pretty bad nerve pain. It has been over 3 months since it started, and during that time I have received an MRI (all clear, except for a couple of schmorls nodes), and tried acupuncture and some therapy exercises.
My nerve pain has been very confusing in that it seems to be following different paths. Initially the nerve pain was almost exclusively a burning pain in my left outer shin/ankle. It would occasionally shift into the arch of my foot. There was no pain or discomfort to speak of however anywhere above my knee. That has changed in the past month however, and now along with the burning in my left outer shin/ankle I now also have some diffuse burning in my left outer hip/glute area that runs into the top of my thigh, as well as a tightness and burning that goes straight down the back of my left leg(sciatica). The nerve pain started when I was doing some self-adjustment exercises in bed for an S.I. joint problem on the RIGHT side of my back that had been bothering me for a couple of months. I did the exercises for both sides. After doing these self adjustment exercise I immediately started experiencing some pain in the LEFT side of my back, I went to sleep, and the next morning I started having nerve pain. Curiously, in the first week, the nerve pain disappeared for a few days before coming back with a vengeance.
I have been reading lately about “gluteus medius syndrome”, as well as “gluteus minimus syndrome”. A quick Google Image search of either of these shows almost the exact path of nerve pain that I have been experiencing for the past month. I wonder if you have any insight into whether these or other exercises may help? I know that I have very strong, and well firing gluteus maximus muscles. I was a regular deadlifter, and my muscles contract appropriately during glute bridges etc. However, I noticed for a long time that my glutes were slightly crooked, and have for the past two weeks focused on building up my gluteus medius muscle through resisted band monster walks, and clams. I have noticed a change in the shape of my glute medius as I have definitely been building muscle through these exercises, and the glutes seem to be “evening out”. However, there seems to be minimal change in my nerve pain at the moment. The pain is at a steady 3/10 that comes and goes, and there is an almost chronic tightness down the back of my leg. Stretching does not alleviate this tightness, and in fact flares up the nerve pain.
I know this is a long, and muddled explanation of my problem, but in truth, it has been a long and muddled few months. My doctor has no clue, my P.T. didn’t either, and neither did the acupuncturist. It seems I have been getting closer to figuring out what is going on through the internet, but I am still stumped. Do you suggest I continue with these exercises for another few weeks and see where that gets me? Any insight into whether this may be gluteus medius syndrome, and if so what I should do about it? Any leads, or even just hunches would be greatly appreciated.
Hi Ellie,
I am unsure if the exercises will help, but the main question that needs to be answered is WHY you have the glute med trigger point syndrome. I’ve never heard the psuedo-sciatic term, but same thing. You explain exactly how it travels on the outside of the leg. And, it is from the glute med. So, is really just that? Or, is your spine sending a signal to that area? Are you not dissociating well? Meaning, is your pelvis, leg and trunk all moving together and they don’t work independently? Are you only recruiting a few fibers of the glute med so it’s become overused (trigger point pain) and the other fibers are just lazy? The answer to your pain is in the WHY. This rarely happens “on its own.” I see it my runners who have no idea that they run from their glutes and core and have limited hip mobility, I also see it with L5/S1 spinal contribution. I hope that helps you solve the puzzle a bit better. If you want to email me to set up a possible skype session so I can watch your movement, let me know! Thanks for your response.
I’m sorry just to amend what I wrote earlier. I did not mean gluteus medius syndrome, but gluteus medius pseudo-sciatica. Apparently this is a condition that causes sciatic like symptoms particularly down the lateral part of the leg into the outer ankle like I do. This can also apparently irritate the piriformis which would possibly explain the pain I have down the sciatic path as well… If I sound confused and speculative, it is because I am. All I have are working theories and little hope :/
Hello, I came across your article shortly after hurting myself by stupidly way overdoing “tennis balling” and stretching my piriformis (it is a long story why I have piriformis syndrome; I had a hip injury a few months ago that caused my glute max and med to become really weak) I know you’re only supposed to work on one spot for 30 seconds but I got carried away and did it for minutes because I had all of these lumpy spots I wanted to “work out”. I’m now really worried that I’ve hurt the muscle and/ or irritated my sciatic nerve. Do you have any advice on what I should do now? Do you think you’re likely sustain any serious injuries from this, or should it get better on its own? Help please!
Hi Kyra,
You should never roll over the sciatic nerve. Ever. So, if that’s what the 30 seconds rule is relating to, please stop. You will need to calm down the nerve. You can try ice (superficial treatment for a deep issue) but it can sometimes help with the nerve signal/pain. The nerve pain will calm down, but in the meantime you need to find a glute max and glute med/min exercise that trains those muscles and does not cause pain. Doesn’t matter what they are. This really doesn’t “just resolve.” It takes some active work to train the right glutes to kick on. Hope that helps!
Hi Lori,
Thanks for all the logical information. I had a couple questions about PS. I believe what you’re saying about hypertrophy makes sense for my case, but I know you acknowledge that there’s a few potential reasons as to why the piriformis could cause someone trouble. In my case my issues started after a weekend of, truthfully, being extremely lazy. After a crazy few weeks of moving states and unpacking, I spent a lot of time in a desk chair, slouched, with my feet up on the desk. With the move, my activity level definitely dropped, and I was no longer cycling and rock climbing like I had been, so weekend glutes definitely make sense. My questions is, does this extended bad posture seem to like up with that as well? Or would you expect that to cause one of the other issues you mentioned? Thanks for taking the time to write this and respond to everyone!
I should add that sitting seems to be the worst thing I can do. When I stand up from sitting at work, sometimes I almost feel a cramping-like feeling, although I’m generally not in pain while sitting. I am however usually in pain while driving, probably because of the bad seating position, and shifting aggravates a little more (manual transmission). Any time I can keep my hip unbent, things usually feel pretty alright. Pain is on the right side.
Hi Andrew,
Great questions. Yes, your weekend of lazy and relaxed posture likely contributed to this because the glutes became “unused.” I would suggest working on true glute activation for 2-3 weeks and see if you get symptom relief. Sitting is usually a worse position for most people with PS, but not always. Work on finding the good glutes and see if that helps!
This all makes sense. After being treated for degenerative disk disease, SI joint dysfunction, and piraformis syndrome with no relief , my new sports medicine doc thinks I actually have ischiofemoral impingement. Do you think the same principle would apply for the QF(?) muscle?
Hi again Beth,
Are you meaning the quadratus femoris (deep muscle in hip in back) or Rectus Femoris on the front? I have actually never heard of the QF being an issue for nerve pain, unless you have some anomaly and your sciatic nerve runs close to it. It’s the sciatic nerve being pressed on that gives this pain, not usually the muscle.
Last time I read this and saw a link to the glute strength exercises you have in another page. I don’t see it now. Please advise. It’s too bad I didn’t see this 8 yrs ago. I saw it after piriformis muscle release surgery. But trying to educate anyone I can on this. Just posted a link on a piriformis muscle support group I found on FB. I told them the exercise link was here, but don’t see it now. Thanks, Barb
Hi Barb, I just saw the link all the way at the beginning area of comments. Look again.
Thank you Chris!
I think Chris let you know before me, but there is also a search bar on the side. Type in “Glutes” and it should pop up.
Hello Lori… wow,,, just now reading your site and forum posts… I had been rolling a tennis ball under my Piriformis periodically for the past 2 months,,, and stopping now, after reading this..bad thing, is I’ve dealt with this for the past 12 years and gotten worse the past 5 years, do to chronic fatigue and sitting and muscle weakness,, I’ve been doing personal research and a common thread is to strengthen the glues and abs, which I am slowly and cautiously doing,,, have to be so careful, as just bending wrong has caused my high hip, Sacrum, low back to lock up ( immense pain ) just had an MRI done, as new chiropractor ordered it, the x-rays showed many things going on with my entire back, before he starts a protocol ( I saw the glute exercises you posted) will they cause any undo stress on my lower back? I am also 62 yr. ols woman. I still do some of the simple Piriformis stretching, which helps only bit temporariy… sitting even at the computer for more than 5 minutes tightens all the hip and thighs up… so I am avoiding sitting period.
Hi Pauline,
The exercise should not cause any back issues or stress IF you do them correctly. Maintain stable pelvis, and isolate leg moving on the body to engage the glute, not the back. Hope you get relief soon.
Hello Lori, I am glad I found your website cos a lot of things made sense.
I think I have piriformis syndrome. 5 months postpartum I stepped funny while holding my baby. After that I started having pins and needles in my foot. That stopped after a month but a pain in my hip started. When I started with massages things just got much worse. Also stretching is making it worse. Every time after tennis ball massages I just feel more pain. My MRI showed a 1mm protrusion but not compressing the nerve. My pain starts in my butt (most painful there) and I feel it in my calf and foot. Manual therapy did not help. This all started about 5 months ago but for the last two months things just gotten worse. Any suggestions?
Hi Uli,
Try to get the good glutes to activate. Since you have ruled out the spine with the MRI, you need to find an exercise for the side glutes (med/min) and back glute (max). That can be fire hydrants, clams, Pilates side series, just sitting squeezing your glutes. The idea is to feel the glutes activate without pain. And…try Pilates 🙂
Thank you for your reply. Have started with those two exercises. I guess it won’t get better over night. I stopped with tennis ball and stretching. You wouldn’t recommend even very light stretches cos now I feel my piriformis tightened and very suttle pins and needles started again in my foot. Or shall I just put up with it until I activate those glutes? Can you please explain how did you get to this insight and why would every single PT reccomend stretches and massage if it doesn’t work?
Hi Uli,
No, no stretching at first. I know that is the sensation, but it is a temporary relief and just continues the cycle. Work on those glutes. How did I get the insight? I am always reading research and trying to think about the body from a very anatomical/biomechanical perspective. Meaning, we are put together really well…why do we complicate it? And, in all of my patients I have found with piriformis syndrome they had really weak glutes. So, the data just starts to add up. Hope you get relief soon.
Thank you so much for your reply. Will continue with exercises and no stretching. I guess I will just have to accept, it will be painful before it gets better. Will let you know how I am progressing. Keep up the good work!
Thank you for your reply. Have started with those two exercises. I guess it won’t get better over night. I stopped with tennis ball and stretching. You wouldn’t recommend even very light stretches cos now I feel my piriformis tightened and very suttle pins and needles started again in my foot. Or shall I just put up with it until I activate those glutes? Can you please explain how did you get to this insight and why would every single PT reccomend stretches and massage if it doesn’t work?
Hello Lori. The 2 exercises are all you prescribe and how many days a weak and how many sets.thanks
Hi Richie,
Well, that is not all I prescribe, but it is the main gist. 1-2x/day 15-20x each so that you create a good Neuromuscular connection and some fatigue in the good muscles.
Hi Ma’am , i am from India I have this pain in my top right butt from 1month.Doctor said that I have piriforis syndrome but no sciatica.I can sit,run,play football and I won’t feel anything significant.but I just know that this pain even though how little it is its not going away..its still there …I am taking antiinflammatory medicines but still no change in the pain.for a day or two the pain became even more less I thought medicines are working but then again this was temporary.stretching is not giving good results.
What should I do next ?
I love playing football(soccer) ..I love running …when will I be able to do this again without this little pain…
Hi,
Yes, you need to be on top of this condition before it becomes really painful. You need to try and activate your glutes. You’ve tried meds, stretching and now realize they really don’t help. Give it a few weeks and find the good glutes to activate. There should be no pain in the exercise when activating the glutes. And, you will be able to run again when you have glutes…we run from those muscles. They are our propellers through space…
Hello Lori,
what about trigger point therapy? Should also stop that?
Thank you
Hi Cara,
Not directly over the piriformis/sciatic nerve area. If they are doing it around the area (edge) that should be ok. NEVER in the center.
Thanks! Have been doing the glute med exercise you posted but can’t seem to find a right glute max for me. Have tried the one you posted and after a few days it was too much for the piriformis. Also tried the bridge and butt squeezing but after a few days it is too much on P again. Seems like P is working a lot when trying to activate glute max. It is annoying. What do you think?
Hi Cara,
Yes, sounds like you haven’t found an exercise to kick on glute max and kick of the piriformis. Bridging usually is not a good choice. Try fire hydrants or just simple glute squeezes on your stomach to see if that helps.
Hi I am 4 weeks into what I think might be piriformis syndrome. Everyone tells me to stretch but this just sets me back and increases the plain. I was also advised the tennis ball but chose not to use it due to all the literatur out there. I am on on co codramol and Naproxen which only makes the nerve pain radiating down my leg to my foot tolerable. I have been doing yoga used to be a runner years ago and I cycle but not in excess. I cant do any thing right now, I was actually getting a little better but I now much worse again after a deep tissue massage. I did have a fall too waking my dog who knocked me off my feet and I fell on soft ground onto the hip that is hurting. At the time I did not notice additional pain from this so not sure if it is relevant. There is so much conflicting information out there I don’t know where to start. I am a slim fit 60 year old worried about the impact on my body because of long term use of medication. My sports massage guy who has helped me many times before said I need to see an osteopath as there is something wrong with my pelvis. The thought of someone cracking my bones makes me shiver. I am in pain and I feel tired and I feel lost the doctors just prescribe pain killers it will be month before they will consider giving me an MRI.. what do you suggest.
Hi,
Try a physical therapist! We also can help with pelvis mobility, alignment (if that is what is truly going on) and nothing is forceful or painful. We do mobilizations, just with less force because the force is not usually indicated.
Hello Lori (from the UK!),
I was going to the gym 5 times a week (a combination of spinning, rebounding, some HIt and things like lunges, squats etc) and back in May, I started to develop PS. I saw a chiropractor who did help but it never went away 100%. I slowly got back into the 5 days a week exercising again and since October, my PS has been a hell of a lot worse. Fr about 2 weeks, I was doing all the exercises that the chiropractor had told me to do before and I suspect I might have over-used the muscle.
I’ve already had 4 sessions with a PT who says I should have a scan if there’s no significant improvement by session 6 to rule out anything else.
He asks me to do these exercises:
– Piriformis stretch
– The Cobra
– Rolling knees side to side.
– Lying on my back, bringing my knee up and lifting my leg up and down
– Pressing my back into the floor
– Pressing my back into the floor and lifting my bad leg and opposite arms a few times
– Standing up and bending backwards.
I’m just so fed up as it feels it never goes away. I am taking gabapentin on a maximum dose and I still get really bad pain sometimes. I do find keeping mobile does help but the first hour is hell. It’s really getting me down as I am an active person and I am getting married in May.
Just wanted to rant, but grateful for any comments.
In addition to this, my PT is doing ‘centralisation’. I think it’s helped as the pain has gone from back of my knee and is now in my upper thigh/butt/lower back. It just feels like it’s taking a long time.
Hi Luci (From the UK!),
Centralization is a McKenzie technique/thought process. And, it really is only effective for spinal contribution of sciatic pain. Have you had your spine ruled out? If it’s PS, only glute activation (not stretching) will change those symptoms. Seriously, all my patients are 100% healed when it is truly PS. If there is a spine contribution to your sciatic pain, different story. If you are getting relief with centralization, make sure you have a clear understanding of what is going on at your spine. IN general, your exercises still need deep abdominal and glute activation to be truly effective. Hope that helps!
Lori, I had a piriformis muscle release surgery last February. My pain returned at 5 weeks post op. Took me 8 months to convince doctors something was wrong. I found a peripheral nerve surgeon, Dr. Tim Tollestrup in Nevada. He did surgery on me 11 days ago. I had instant relief. He has a high success with his method. He modified the retractors he uses so he can see more. He found the muscle that had been released grew back with scar tissue to the nerve. He also was able to see I had a complete second piriformis muscle with a split siactic nerve. He said he has seen this before but a rare occurrence. He removed both muscles.as you said in your blog, this is an assist muscle. I have no issues with movement and have already started therepy. I believe I made the connection with my timeline of this condition when surgery was needed. Six years I had this and controled with therepy, chripactior off and on. When my pain became chroinc, scar tissue had set in and I reached the point of no return. That was two years ago. In my research I found the surgical release surgery is not very successful.recurret piriformis syndrome is high. This newer Tollestrup method is very successful, if the pain gets too bad.
Hi Barbara,
Thank you for your personal insight. Yes, I always say there is a time and place for surgery, but it should be the very last option. It sounds like you tried everything conservative instead of going for the knife first. So happy you are having relief!!
Lori,
I have had a sit down job of 9-10 hours a day for 3 years now, which I think has led to piriformis syndrome. Now it is painful no matter whether I am sitting, standing, or even laying down. I have been doing the 2 glute exercises you recommend, although not daily. My question is – will I be able to heal and still sit so many hours a day? If need be, I will quit my job. I am also debating going to a physical therapist, as I want to treat this naturally and not waste time & money on something that won’t help.
Hi Joy,
I would definitely recommend seeing a PT. No, you do not have to quit your job. And, yes, it can heal once you find those glutes to give stability with sitting and not piriformis. But, make sure someone clears your spine first to make sure your pain is not stemming from there.
Hi Lori! I just wanted to report back with some positive feedback. I have a bulging disc that got irritated due to a twist and lift accident and it made my left side develop compensation patterns and the piriformis was the cherry on top of everything eventually breaking everything down and making even walking to the bathroom a terrible experience. Since I was so far gone it took a long time but I can confirm here for everyone that it is possible to come back. It’s not gonna be easy and requires a lot of discipline and you will feel up and downs but if you stick to your exercises and avoid stretching to no further irritate the piriformis it will go away! Besides the clams and hydrants that you recommend I found a program specifically designed for the piriformis which includes these two exercises to get started but then gives further exercises once you mastered these. It’s called the Powers program named after the professor who put it together and it was a life saver to get me back to action. I thought I leave the link here if anyone else is interested if that’s okay. It took me all in all about 6 month, but like I said I have some other issues going on to. Stay strong everyone, there is hope!
http://www.sportsandortho.com/UserFiles/POWERS%20-%20ALL(1).pdf
Hi Paul,
Glad you are feeling better. I usually don’t allow links on my blog, but I do respect Christopher Powers, Phd, PT and his philosophy of loading tissue (ie. the glutes in this case) is the same as mine. His program is very similar to those I use in the clinic. For those reading: you must master finding the glutes before you even consider weight bearing (ie. step ups, lateral lunges). Thank you Paul!
Hi Lori,
I’ve experienced chronic pain in the right buttocks/hip for several years now. It was determined that I had a labral tear and had surgery to repair about 1.5 yrs ago. However, it didn’t solve the issue. i’m a sculler and am currently sidelined due to pain + muscle spams up the right side of my back. I’m in PT right now for SI/Piriformis treatment (clams + other ex) but nothing seems to help. I’m trying to maintain some exercise (spin cycle) and lifting weights on upper body. Do you recommend ceasing all activity except for prescribed exercises until injury calms down? I’m feeling quite hopeless right now as this has been chronic for so long. The, Dottie
Hi Dottie,
No, lack of movement is not the answer. You need to stop activities that bother your R glutes/hip, but not everything. If you are not getting relief, those glute exercises are not for you. Have your PT figure out some glute exercises that stop your pain and kick on the good glutes (that should happen at the clinic with her).
Hi Lori, thank you for being so helpful and sharing your information. You’ve reached Scotland,UK now!…I was hoping you could help me please – I’m 34 and had PS for over 2 years (no injury-just came on one day), been to many specialists and had steroid injection to piriformis in the last few weeks which has eased things greatly. I’m using this relatively pain free time to work on building up glutes and ensure they are activating (Chiropractor said they weren’t but then would on a slight pelvic adjustment) I’m doing hip flexibility exercises and your clams and fire hydrant but my painful side doesn’t have a great range of motion during clam (about 4 inches less travel between knees than right) – it feels like muscles near hip are solid and leg will not travel any further. Is there anything that would help this or will this not be a problem? Thank you!
Hi Colin,
Try doing the clams with your feet off. So, same position, but keep knees down and lift heels off. That should improve your range of motion.
Hi Lori! I am so pleased to have found this page with loads of good info and am eager to try out your tips. About 6 months ago, I heard a loud and distinct POP while doing “compass” pose in yoga, and have been dealing with PS ever since. I’ve continued my regular yoga practice, which is limited since the injury, and it seems to irritate and even cause pain in my bum and back of leg. The elbow digging and tennis ball have been my only relief!
My question is regarding EMS and/or TENS, which have been briefly mentioned in this thread, but I was wondering if you feel that either one of these therapies, used regularly, would help ease the pain (or cure the problem)?
Also wondering if there is any risk of further injury if drug therapy (anti-inflammatories, steroid or botox injections) is used to block the pain, and I can’t feel how far or deep into a stretch I should go when practicing yoga.
Hi Megan,
TENS is just a fancy bandaid. There is no healing power to tissue, it just disrupts the pain pathway (which is not harmful). So, if the TENS helps you sleep or work with less pain, go for it. But, it’s not actually solving the problem. I would stop all stretching to the area in yoga except sitting in criss-cross and leaning forward. It is safe to stretch this area if the sit bones (pelvis) is grounded on the floor. No pigeon. I don’t suggest injections in this area, but you can see if Ibuprofen would help. Try working on more glute activation and less stretching.
Thank you very much for your reply. Time to get the glutes going!
Hi Lori!
I just came across your site and found this page really helpful! I’m a 27 year old female and a few months ago I hurt my lower back while doing ab exercises on a bed (genius I know). I went to PT for it and the therapist told me to do clams to help eliminate the pain. After a couple months the back pain went away and I wanted to take my exercises further so I added a resistance band to my clams. I was trying to concentrate on keeping my hips parallel to the wall in front of me in an effort to create more resistance for my glutes, rather than fully opening up my hip which has always felt more comfortable in a turned out position during work outs. Looking back this was stupid and maybe too much too fast or just done with the wrong form because I now have PS. How can I make sure I am activating the “good glutes” and not compensating with my piriformis? Thank you!!!
Hi Ashley,
If you are using the good glutes, you won’t feel that nerve pain. It will feel like muscle fatigue pain. When most of my patients first find the glutes again, they do shake a bit. This is just neuromuscular “talking” that is happening. Hope that helps!
Thank you so much for this info. I’ve had so much pain in my left buttocks, sciatic pain and now I believe I have Piriformis Syndrome. Had epidurals injections them seemed to help but only for a short period. This pain affects my entire left side below the hip and plantar fasciitis is a constant struggle. The other night my husband pointed out that the upper region of my glute was sunken in. As in it’s atrophied. Sort of in a panic now. I’ve lived with this pain for a long as I can remember and I willing to just deal but since it’s actually affecting me on the outside, I would like to fix it and get some relief. What kind of doctor do you recommend? And I’ll be sure they understand I’m not interested in masking the pain but in determining exactly where it’s coming from and correcting that. Thanks again.
O and I should probably note that I also have a herniated ruptured disk in my low back.
Oh, well…you need to go see a physiatrist (MD) to see if that disc is causing muscle atrophy in other areas of the body. Or if you have muscle atrophy because you just stopped moving well because of pain. Two very different things.
You need to go see a physical therapist, not the MD. You need someone who will teach you how to move your body well again, not prescribe pain pills or a surgical procedure.
I have sudden piriformis flameup and sciatic compression. I believe what you have written makes sense in my case. I believe the flare up to due to suddenly using heavy weight on one of those hip abduction resistance machines (sitting with hips and knees flexed 90 degrees). My guess is at very high weight, I am suddenly recruiting the piriformis hmuch more than normal. The worst pain came ~3-4 days later, which may indicate hypertrophy, or at least higher tension.
Ironically I had some similar hip issues before, and I felt my glut med was weak. I thought the machine would help, but it didn’t. Then I worked on exercises like the fire-hydrant and that solved it. So I could see the strenghening of the other glute muscles being important and sufficient, so long as I don’t do any exercise with enough weight to stimulate the piriformis to hypertrophy!
Hi Joe,
True hypertrophy takes 8+ weeks. But, you may have been using that piriformis more than you think if it was that easily flared onteh machine. Honestly, I am not a fan of that machine because it does not train the glutes in a functional, optimal position. You are better off with lateral lunges, band walks for hip abd strength. But, you seem to have a hang of what caused your pain. Find glute exercises that do not cause pain, just good glute activation.
Hi, I’ve been suffering from what I think is piriform syndrome with sciatica down my leg. I was told 7 months ago it was a herniated disc but MRI negative. I found a physio who discovered that I have an extremely weak glute muscle so he started me off on donkey kicks, bridges, then one leg squats, which seemed fine at first then really irritated the bum muscle and made things worse. I also went to a pain management doctor who assessed me and agreed it is piriformis. He found also that my bum muscle is very weak but after releasing the piriformis my gluteal was activated and strong, temporarily. And i do find that when I do my exercises that bum miss.e doesn’t seem to work properly. So, my question is how the heck do I activate the gluteal muscle to strengthen it or is it just a matter of stretching the heck out of the piriformis to keep the glute activated because it really is already strong? Or do I just keep doing bum exercises in the hope that the gluteal muscle will overcome the piriformis? Right now I do donkey kicks, bridges, clams, and a few others. No real improvement. Thanks for any advice yu can give me. Tina
Hi Tina,
Do not stretch! NO, no, no. Biggest mistake and greatest piece of misinformation on the internet. You need to start with lower level glute exercises. The ones you mention require some real strength from the glutes. If they are weak, guess what takes over? Other stuff…especially Piriformis. Please watch Blog Talk: Piriformis Syndrome. At the end, I demonstrate a few easy exercises to kick on the glutes. Hope that helps.
Thank you so much for replying. I have started doing the exercises you suggested-clam, fire hydrants, leg lift with circles. Is there another exercise that one can do instead of fire hydrant? i think it is bothering either my piriformis and/or my back. Or maybe I am doing it wrong. I see a new physio tomorrow, so am hoping she is into exercise therapy and is knowledgeable about this syndrome. Otherwise I may just drive to Colorado to get a consult from you! Only half joking–I am in Canada.
Hi Lori, Thanks so much for this – it makes a lot of sense. After 30-plus years of running, I started getting nagging butt and upper hamstring pain on my right side almost a year ago. I ended up getting an MRI, which was basically normal, so the assumption is that it’s my piriformis. I finally hit pause on running a couple of months ago and switched to biking, and I’ve been working on improving my core and glute strength. (I bought your pilates glute video and have started doing that regularly.) It’s been a zigzagging, often confusing road but I think things are (hopefully!) starting to slowly get better. One thing I’m wondering: I have significantly less glute med/max muscle mass on my bad side than on my good side. Should I still exercise both sides or does it make more sense to concentrate on my weak side with things like single-leg bridges and single-leg squats? Thanks again!
Hi Josh,
Yes, exercise both. You may do two sets on the bad side and one set on the right. But the good side will neurologically teach the bad side what the movement normally feels like. Glad you are on the right track now with glutes!
Thanks for clarifying that. The thing that’s so crazy-making about this thing is that progress is not in a straight line and what causes a flare-up is often unclear. (And it doesn’t help that there is so much conflicting, often totally contradictory advice out there on how to treat PS!) But I’ll keep working on turning on the good glutes and try to keep the faith!
Hi Lori: I have read a lot of the comments and issues that have been posted here about piriformis syndrome. I pulled a patient up in bed 2 summers ago and felt an electrical zing go down my leg. Ever since then, I have been in pain. I went to PT X3 and a physiatrist, all seem to think this is piriformis syndrome. I have been dealing with this for 2 years and am very frustrated. I do my exercises every day without fail which includes clams, one legged bridges, side leg raises, and stretches. When I do clams, my nerve gets activated and starts to tingle. Do you think I should do clams even if my nerve gets active? Do you think this will ever heal? Have you heard of botox used to paralyze the piriformis to help calm the muscle down? I have read that botox coupled with PT could make a difference. What do you think?
Hi,
Well if you feel the nerve with clams, it’s not your exercise. It will heal, but you need to find glute exercises that don’t hurt and just isolate the good muscle tissue. If you go to Blog Talk I do give a few other exercises that might help. Don’t feel pain with the exercises!! https://www.youtube.com/watch?v=xp-0TteiyO8&t=212s
Hi Lori, have read your article with great interest. I am not sure how long I have suffered from piriformis syndrome as was not diagnosed and mis diagnosed for so long but has been at least two years. I have been doing 1-1 Pilates for about a year now which has helped stablise and strengthen me as my original problem way back was that my pelvis was tilted to the right. Then last June I bought this bit of home exercise kit called a Legmaster – think it is Legmagic in the States – I am in UK – which itargets your inner thighs whilst standing and drawing legs in and out on a slightly curved platform and within literally days, I was better. My inner thighs were aching like mad to start but everything else stopped hurting and I had about 3 blissfully pain free months feeling like a normal person again – it was like a miracle! Then I drove to Wales in October and even though I broke the journey up, it was a good 6 hours each way of driving and I haven’t got back to where I was since. The prolonged sitting obviously aggravated my piriformis and the Legmagic hasn’t worked its magic again. I just wondered, as you sound so much more insightful and skilled than any of the many professionals I have seen here, if you might have any idea why it worked and why it isn’t working now. The machine does hit your glute meds a bit too which I expect is a factor – I do need to work on mine obviously. I have a problem with clams. There is something wierd going on with my rectus femoris too which hurts a lot if I do certain movements. I’m sorry about length of question but if you were able to respond, I would be so grateful – it really is ruining my quality of life. Many thanks.
Hi Kate,
Yes, Piriformis Syndrome can be stubborn. Sitting – it sounds like you do not have enough glute max (the back glute muscle) development. If it is not strong and developed, sitting will always aggravate it. You still need glute med/min, but that back muscle is key to getting that to go away forever. Hope that helps!
Hi Lori, very interesting reading. I sit a lot for work and have been in pain recently with my back and pelvis. Sitting definitely aggravates things. Currently doing clams and glute stretches as advised by my PT. I also tried foam rolling few times which was excruciatingly painful – left bruises. I now have numbness and tingling whenever I sit, literally can’t sit for longer than 5 mins. I am waiting for an MRI. Do you think the foam rolling has caused this tingling, numbness to start? No one seems to know what it is. Appreciate your feedback as it’s causing me a lot of distress. Thanks in advance.
Hello Lori,
I have suffered with PS for ten years now:( I feel as though I have tried everything. I was told by a strength coach that I have weak Glute Med and Max and gave me corrective exercises to try. The first two weeks I felt great and felt like I had a turning point. Ten years of Physio, Chiro, Massage and no one could properly diagnose me. After the third week I am having a crazy flare up and sciatic pain through the roof! waking me up at night and i’m not sure if I should continue with the exercises. I am so at my wits end. I feel the most pain in my PM, TFL and IT band. I’m not sure if this is all a part of my healing but I would love to get your opinion.
Hi Rayann,
Thanks for reading and reaching out. NO, those are not the exercises for you. When you are healing PS it is important to find glute exercises that do not flare anything. You only feel them in your glute. You may need to start with a simple one that helps your brain organize a bit. Lay on your stomach and squeeze your glutes together BEFORE your hamstrings. The hamstrings should always be second.
Hope that helps!
Hi Lori,
Could you list some of the common reasons why the glutes becomes so weak that the piriformis takes over their function. Along this line, you’ve mentioned that runners and cyclists often have weak glutes? Can you explain why that is?
Thank you!
Hi Allen,
Sure! We sit. In chairs, cars, planes most of the day. Sitting in a chair is not functional sitting and the glutes have to do absolutely NO work. Cyclists – usually don’t understand the power production from the glutes and are quad dominant. Runners – usually don’t have great technique and do not propel from the glutes but have very upright running that makes it quad dominant. Does that help?
Hi Lori,
I am a 19 year old girl suffering from Piriformis Syndrom,
I can’t even tell when it started.
I was a dancer 2 years ago until I injured my knee.
After that I was resting for about 6 months and I guess I jumped into exercising way too fast.
Now I have a deep pain in my left glute and My hips and sometimes it goes all the way down to my knee.
Im having this pain since 3 months now
I tried stretching ( helped a little, but not really ). I tried resting it and doing nothing for a month but every time I tried to do something the symptoms would reoccurr
Every time I exercise my glutes( bridges, fire hindrants, clams) it feels worse and I feel the pain even more.
HI Valerie,
You likely need calmer movements to engage the glutes. They are likely aggravating it. Standing and squeezing your glutes together is a place to start. If you want more help with an online consult, email me at [email protected]
Hi Lori,
About two years ago, my leg began getting weak when trying to do my daily walks. I began having extreme fatigue down my leg to my foot, starting from my butt. I postponed having it looked at due to an arm injury from work. I tore my distal bicep tendon. I had surgery to repair it and didn’t want the scheduling nightmare of juggling OT and PT. I knew that was going to be the first thing they tried. Long story short. I had a gluteus medius tendon tear anterior two thirds and retracted. Bursitis, bone spurs, Labral tear and CAM type impingement. I had it all repaired. Seven weeks out from surgery, I fell on the repair. My surgeon ordered me back on crutches to let it cool down. It was very painful. We did not do an MRI because it was still too soon after the surgery to tell if there had been any damage. I have been doing my PT exercises to regain my strength in the glute, but it enflames the piraformis, and after the fall, the whole problem with walking came back. Pain down my leg to my foot. More like a deep ache and extreme fatigue to the point that I have to stop and rest the leg for a few minutes before continuing on. At this point, the surgeons next step is to have an MRI on my spine in case there is an issue there with sciatica. I’m waiting for that appointment. I feel as if I am damned if I do and damned if I don’t. I need to get the strength back in the glute, but at the cost of a lot of pain to the piraformis. I wonder if it is damaged and had been overlooked or perhaps hypertrophy? Any thoughts?
I was wondering if there is a connection between piriformis syndrome and pain on the outside of the shin just below the knee? I am dealing with a combination of piriformis syndrome and IT band syndrome and my main points of pain are the left glute and the outside of my left shin. I used to have severe pain on my lateral knee (the IT band diagnosis) but that has gone away after months of PT but the glute and shin pain still is lingering?
Hi Sammy,
The outside of the shin pain is almost always a referral from TFL (tensor fascia lata). If the glutes are dysfunctional then our body tries to use piriformis and/or TFL to do the work. So, yes, they could be connected. Find those healthy glutes!
I am having similar nerve pain. Down my lateral thigh, skips over knee, and then down the lateral side of my shin. I was diagnosed with piriformis syndrome but I am unsure of this diagnosis because of where the pain is. I have been doing all my stretching religiously and no pain relief. Actually after stretching it seems to aggrevate the nerve and make it worse. Should I get a second opinion, could it be MP? It feels like it starts in the glute med and then runs down laterally. Any help you can give me would be greatly appreciated! I am getting desperate.
Hi Kristen,
I apologize I missed this comment. If it is on the outside of your leg you will want to clear the spine BUT it could also be something I term psuedosciatica. The TFL and glute med/min (if dysfunctional) can create pain down the outside of the leg.
Hi Lori, I’ve had a SI joint issues since giving birth almost two years ago, had extensive PT and chiro (was amazing and helped immensely in addressing a pretty decent leg length discrepancy). Recently I’ve gotten back into running in the past six months and having piriformis issues on my left side, also my weak side, which is causing my right si joint to hurt for some reason. I’ve been laying off my glute exercises (I was doing intense glute workouts three to four days a week to stabilize my joints and wanting to run and possibly overdoing it). Now I’ve been doing gentle stretching for the piriformis the past several weeks, but it’s still nagging and not really getting better, only feels better well after my runs and with heat. Any suggestions for either of these lingering issues?
Hi Kathy,
Go back to PT! It sounds like your SI is doing the running for you and stretching is usually not the answer. There is a probably some “off” firing of the glutes/core for the high function of the run. And, make sure you are doing stability glute exercises (ie. Pilates) not just lunges, bridges, squats. Hope that helps.
Hello. This is a God send. The info here has encouraged my heart. 9 mo ago my foot felt weird and wasn’t working. Went in, got told it was actually herniated disc/ sciatica. Struggled 9 mo. Leg still had sciatica. Finally got MRI… it was perfect. Nothing wrong with lumbar spine. So I’m suspecting piroformis is cause sciatica due to tight, painful spot in my butt. Will strengthening also help get rid of sciatica, caused by piroformis? No one ever answers the sciatica part. Thank you!!
Hi Jess. Theoretically, yes. If you take that pressure off the sciatic nerve by activating the correct glute muscles then that pain should go away!
Thank you so much! That gives me so much hope!
I now use lacrosse and acu-hump to massage my butt for piriformis release. What else can I do to help that?
I am just stumbling across this blog after YEARS of pain and no answers. It started out as what I thought was bursitis in my right hip. Everything seemed to line up and I even got one or 2 cortisone shots for it. However, it has never gone away. Now, I have the feeling as though I am sitting on a tennis ball when I am driving especially, right under my right buttocks. My hip always hurts- especially on the outside hip joint, so bad that I cannot sleep much on my right side as it will throb down my right thigh. Recently I was told by my massage therapist that I have PS and you are right in that pressure hurt terribly but seemed to help briefly. My muscles are SO tight that stretching is sometimes torture and I cannot do things like clams, hip abduction, etc b/c it flares my right thigh up too badly. I was strength training and doing glute work but cannot say it fixed this b/c it didn’t. I don’t have issues in my foot but cannot walk super long periods or my hip will THROB. Any ideas b/c I am at a total loss. I had an MRI of my pelvis which oddly didn’t show bursitis or a labral tear. The only thing I can remember is I think this all started years ago with kettle bell swings and having pain after that. But that has been so long ago and I do think it was the starting point. I am just not sure what to do. I am in VA if you have any suggestions on practicioners as well! TY!!