The X-ray is normal. The MRI is negative. Every doctor visit leads you to more confusion and less answers as they say: “I’m not sure why you’re in pain.” So, they move you along. Not because they don’t care, but likely because they may not know. If the diagnostic tests, medical screens, blood work-up and imaging are all normal, why in the world are you in pain? From the doctor perspective, you look perfect. From the physical therapy perspective, it’s time to consider the bones, joints, ligaments and fascia and how they MOVE. Your pain may be muscle atrophy.
After 11+ years of treating patients, most unexplained body pain is usually muscle atrophy.
***Note: These cases of unexplained body pain have been cleared by the MD for anything significant or substantial.***
What is Muscle Atrophy?
Muscle atrophy is the loss of muscle bulk, size and girth because of poor activation. Clinically, it is known as muscle wasting. Atrophy is MUSCLE WEAKNESS to the Nth degree! Look at the picture below. Notice the difference in muscle size compared to the other. The left calf shows muscle atrophy.
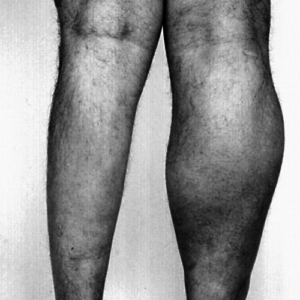
Ok, so what caused this muscle atrophy or muscle de-activation?
Muscle atrophy can occur for several reasons, but the main categories are:
- Neurologic – the muscles receive less or no neurological signals from the brain or spinal cord region. This occurs from compression of the nerves at the spine, a neurological disease or from a significant neurological trauma such as spinal cord injury.
- Non-use – the muscles to do not receive a healthy nerve signal to do their job. Thus, they become unused. This occurs with pain, injury and movement compensation. This type of muscle atrophy will be the focus of this blog.
With pain or injury, most of us avoid movement in that area. And, further, the dysfunctional movement we use to “push through the pain” is muddy and unorganized. (Remember, movement in the body is a direct reflection of what is going on in the brain). After weeks, months and sometimes years of poor movement, the pain in your body starts knocking at your door:
“Please pay attention to me. I’m not well!”
Nerve Signals Move Muscles
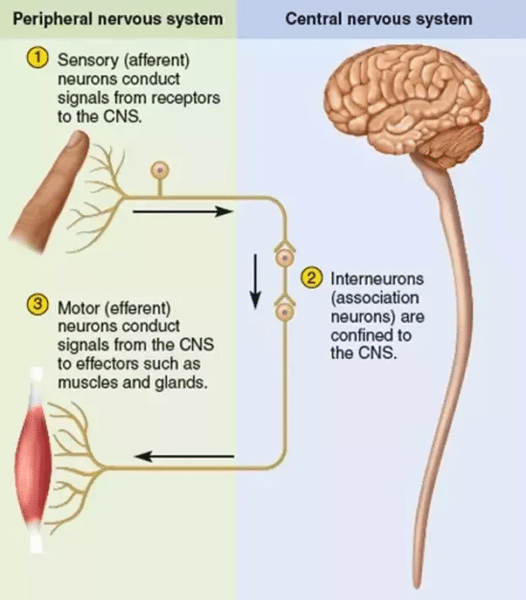
Image from Quora.com
Muscles and nerves communicate with each other. We have afferent nerves (nerves that take signals TO the Brain or CNS) and efferent nerves (nerves that bring signals TO the Body).
Here’s an example. Let’s say you stub your pinky toe on the corner of the wall. Now, that little pinky toe is really painful. A pain signal travels along the AFFERENT path TO the BRAIN and says:
“Hey there! I stubbed my toe down here. Kinda painful. Can you not walk on the outside of my foot. Thanks.”
Your brain answers and sends a message down the EFFERENT path TO the FOOT that says:
“Sure, I’ll have you hop on the other leg or walk on the inside of that foot so you don’t have to make contact with the ground where you stubbed the toe. I got you!”
Within seconds, you are limping or hopping and breathing in air through your teeth. You’re in pain! Thus, you avoid the outside of that foot until the pinky toe pain calms down.
Personal Story: When I was training for my Half Ironman in 2015, I stubbed my left pinky toe 3 times in one day. So ouchy! Running was not pretty that day. Luckily, I was smart enough to stop, come home and ice before I became a dysfunctional mess.
This is how it all begins. Pain occurs, we avoid using a specific area and a cascade of events follows. Muscle atrophy doesn’t happen after a day or two, but if the avoidance of that muscle or body region continues for months to years, then atrophy is the likely result. That makes sense, right? If you avoid using a muscle for long enough, the muscle tissue will decrease in size because of the lack of healthy nerve signals. Gradually, the muscle avoidance becomes muscle atrophy.
Why is Muscle Atrophy Painful?
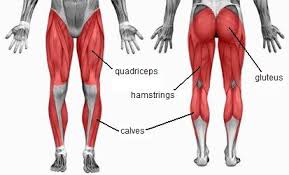 If a muscle is not getting healthy signals from the brain to move and activate, something will take over. For instance, at the hip area, the quadriceps, hamstrings and/or back like to take charge for the glute muscles. At the shoulder, the upper trapezius (big shoulder/neck muscle) loves to act as a scapular (shoulder blade) stabilizer. Neither of these muscle compensations end well. Pain and dysfunctional movement are the end result. And, the end result is a very painful myofascial syndrome (myo= muscle, fascia= connective tissue).
If a muscle is not getting healthy signals from the brain to move and activate, something will take over. For instance, at the hip area, the quadriceps, hamstrings and/or back like to take charge for the glute muscles. At the shoulder, the upper trapezius (big shoulder/neck muscle) loves to act as a scapular (shoulder blade) stabilizer. Neither of these muscle compensations end well. Pain and dysfunctional movement are the end result. And, the end result is a very painful myofascial syndrome (myo= muscle, fascia= connective tissue).
After months to years, the myofascial syndrome manifests into muscle atrophy pain. Now the weak and wasting muscles are actually tender to the touch. But, maybe it’s NOT the muscle that is painful. Likely, it’s the fascia elements around the muscle and its fibers. Fascia continues to be heavily researched. It’s characteristics, properties and capabilities are still being explored and quantified. However, we do know that fascia has nociceptors (pain receptors) that contribute to pain. So, if the glutes are lazy and they don’t want to work, yet the hip requires more stabilization than the hamstring and quad can deliver, what is your body left to use? Fascia. Connective Tissue. Yes, now your brain is really confused and unorganized and trying to use fascia for muscle activation.This is HIGHLY dysfunctional. And, painful.
How To Fix Muscle Atrophy from Non-Use
This is one of the easiest answers: MOVE THE MUSCLE. Activate it. Give it healthy signals. Re-organize your brain. One of the best ways to do this is with a physical therapist who understands the underlying cause of the initial pain (remember, that could have been a few years ago) and can help you re-activate your body with healthy tissue loading. Don’t waste your time with a non-medical provider. Seriously. Go See a Physical Therapist!
A Patient Story of Non-Use Muscle Atrophy
 In the Fall of 2017, a 45 year-old woman was referred to me with unexplained low back and hip pain. Two years before, she had fallen at work. She was highly compliant with PT, chiropractic care and massage through her Work Comp benefits. After 2 years of minimal improvement, the Workers Compensation System no longer believed her pain story and, thus, her case was settled out of court.
In the Fall of 2017, a 45 year-old woman was referred to me with unexplained low back and hip pain. Two years before, she had fallen at work. She was highly compliant with PT, chiropractic care and massage through her Work Comp benefits. After 2 years of minimal improvement, the Workers Compensation System no longer believed her pain story and, thus, her case was settled out of court.
Yet, at her initial evaluation this is what I wrote from her subjective statement:
” My MRI was negative for the hip and spine, but I only feel 65% of normal. I want to sit, work and walk without pain.”
She also stated a nagging “stretch” sensation in her left hip. After telling her history and beginning the evaluation, it was clear why she was in so much pain. For one, her left pelvic joint was significantly rotated, causing a “stretch” sensation to her hip. However, the most memorable finding was that every single tissue along her low back, left glutes and hamstrings were extremely tender to light touch. I was barely touching her, yet her pain was reflexive, reactive and high. Her connective tissue was trying to stabilize, move and do the work of the lazy glutes and leg muscles. Her muscle atrophy pain was the very end result of her pelvis getting rotated after the fall. Talk about a cascade of events!
Her 1st Treatment: neutral core activation, side glute lifts with a band for assistance, leg/pelvic dissocation. 4 exercises. That’s it.
After 7 treatments in 2 months, she stated she felt 90% of normal.
If you really listen to the patient, they will tell you exactly what is going on!
This blog post is dedicated to CM…a very special patient who inspired and encouraged me to write about this topic.
© 2018 and Beyond. ALL BLOG CONTENT at duncansportspt.com by Lori Duncan PT
***Update February 2019***
BLOG TALK PODCAST
Unexplained Body Pain: Muscle and Fascia [1]
ABOUT THE AUTHOR
 Lori Duncan, DPT, MTC, CPT is a respected Physical Therapist, Manual Therapist and Pilates instructor in Lafayette, CO. Lori is passionate about preventive physical therapy and education and is a nationally recognized presenter. She can be reached at [email protected]. You can also follow Duncan Sports Therapy + Wellness on Facebook [2] & Instagram [3] for more free tips and information.
Lori Duncan, DPT, MTC, CPT is a respected Physical Therapist, Manual Therapist and Pilates instructor in Lafayette, CO. Lori is passionate about preventive physical therapy and education and is a nationally recognized presenter. She can be reached at [email protected]. You can also follow Duncan Sports Therapy + Wellness on Facebook [2] & Instagram [3] for more free tips and information.
References
Willard FH, Vleeming A, Schuenk MD, Danneels L, Schlep R. The thoracolumbar fascia: anatomy, function, and clinical considerations. J Anat. 2012:221;507-536.