Knee Arthritis: Does Running Really Make it Worse?
If this question was asked 20 years ago, the quick and common answer would be “YES”. Intuitively, it makes sense that running would increase arthritis. If you consider the contact of the foot on the ground, over and over, for miles and miles, the wear and tear seems probable. Luckily, research continues to find that running does NOT progress knee arthritis. For those of you who love to run, happy news, right? If running does not progress arthritis, what are some of the factors that do? You may be shocked to know…
What is Knee Osteoarthritis (OA)
- Osteo= bone
- Arthritis= inflammation
 It is inflammation (swelling) of the bone at the knee. In healthy knees, there is a layer of cartilage (smooth, silky stuff) that covers our bones at the joint. This allows our joints to move without pain. But, if that cartilage somehow gets damaged or starts to wear down, bone is exposed. Exposed bone = pain in the joint.
It is inflammation (swelling) of the bone at the knee. In healthy knees, there is a layer of cartilage (smooth, silky stuff) that covers our bones at the joint. This allows our joints to move without pain. But, if that cartilage somehow gets damaged or starts to wear down, bone is exposed. Exposed bone = pain in the joint.
Let’s say you have a little OA in your knee. Your doctor has told you it’s minor and not to worry about it. Maybe you’ve even been told not to run. Well, you might want to bust out those running shoes, but it would be advantageous to find out if you have any of the following on the list.
Top 4 Predictive Factors of Knee OA Progression
1. Baseline knee pain
Yes, simple knee pain. Pain with stairs and squats, but maybe not with walking or at rest. Knee pain is a HUGE indicator that your knee will progress down the arthritis lane. And, this is one of the most easily addressable items on the list. I always tell my patients it’s not normal to have pain in your body. Maybe some stiffness as we age, but not pain (injury and surgery aside). Unfortunately, so many people are functioning with unexplained knee pain and don’t think it will ever get better. Please, please. Go see your local physical therapist. Knee pain is not normal; halt the OA progression.
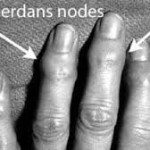
2. Heberden’s nodes
Heberden’s nodes are specific to the hand. Arthritis attacks the joint closest to the fingernail (called the DIP joint). This arthritis or swelling forms a bony mass of tissue, making the joint look bigger and even displacing the fingernail off to one side. Unfortunately, genetics is the main cause of these nodes.
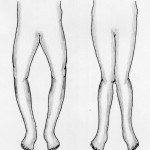
3. Varus alignment
Also known as: bowlegged. Again, mostly a genetic predisposition, but there are exercises and movements that can help halt the “extremeness”of the bowlegged alignment.
4. High hyaluronic acid levels
Hyaluronic acid is a type of GAG (glycoaminoglycan) found in the ground substance of cartilage. Simply, it is a protein that loves water and is able to keep cartilage supple and pliable to resist compressive forces in the joint. However, extra high levels of this acid is a signal of joint inflammation. This is a conversation with your medical doctor and a blood draw.
Conflicting Risk Factors for Knee OA Progression
This is a long list (and not all-inclusive) that requires more research. Some studies show these factors do increase OA progression, some don’t. But, the list below is worth noting.
- Low bone density
- Insulin levels
- Valgus alignment- knock-knee (opposite of varus)
- Presence of OA in other joints
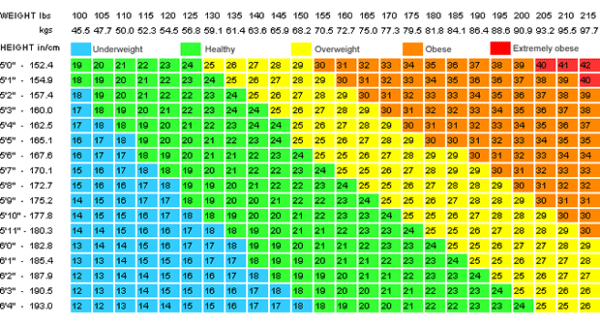
- BMI– Body Mass Index. BMI is a poor indicator of body composition or body health. A very strong, muscular individual can land in the overweight category on the BMI scale. On the other hand, a thin, weak person will be considered healthy on the BMI. Here’s my point. You need muscles to function, so find your muscles. Who cares about the BMI. I will say this: the less body mass you have to move through space, the easier it is on your joints. But, it’s finding the happy medium. Good strength with a good weight.
Top 5 Factors that do NOT predict Knee OA progression
1. Sex
It does not matter if you’re male or female
2. Previous knee injury
Just because you have injured your knee in the past doesn’t mean you’ve set it up for failure. Just rehab it well so you don’t end up with some baseline knee pain. Because then you leap to the list above and that’s not awesome.
 3. Quadriceps strength
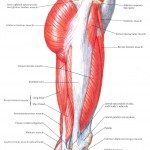
3. Quadriceps strength
The quadriceps is a set of 4 muscles on the front of the thigh. These muscles extend the knee (make it go straight). One research study did find that increased quadriceps strength on a loose or mis-aligned knee did increase OA. But, that’s only because the knee was getting an extra strong pull on the front. Remember, it’s important to balance the body by strengthening everything! This includes: hamstrings, gastroc, soleus and those wonderful glutes I’m always yappin’ about.
4. Smoking
But, please don’t start smoking a pack a day thinking it’s good for you!
5. Running and regular performance sport activity
Main Take Home Point
- If you have any baseline knee pain, get it checked out. This is one of the main risk factors for knee OA progression and one of the main things most of us will ignore.
Thank you for reading! ~Lori Duncan PT
 If you enjoyed this post, please share! If you or anyone you know are in need of physical therapy, please contact me.
If you enjoyed this post, please share! If you or anyone you know are in need of physical therapy, please contact me. - Subscribe to the blog with your email. You will only receive an email when a new post publishes.
References
Bastick AN, Belo JN, Runhaar J, Bierma-Zeinstra SM. What are the prognostic factors for radiographic progression of knee osteoarthritis? A meta-analysis. Clin Orthop Relat Res. 2015;473(9):2969-89.



excellent read, thank you… age was not mentioned….is this a factor? I am 74 female 120 lbs 5’4″ and walk/run on a treadmill for 40 min 2-3 days a week…lately having shooting pain in one knee (the good knee, the other had Orthoscopy surgery 6 year ago)….I thought the colder weather may be a factor. I started tumeric also. thank you pb
Hi,
I think your regimen is just fine for 74. If you are feeling sharp pain I would not ignore that. Could just be soft tissue (tendon/ligament) but make sure you stay on top of that.